

SUBSCRIBE TO OUR FREE NEWSLETTER
Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
5
#000000
#FFFFFF
To donate by check, phone, or other method, see our More Ways to Give page.


Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
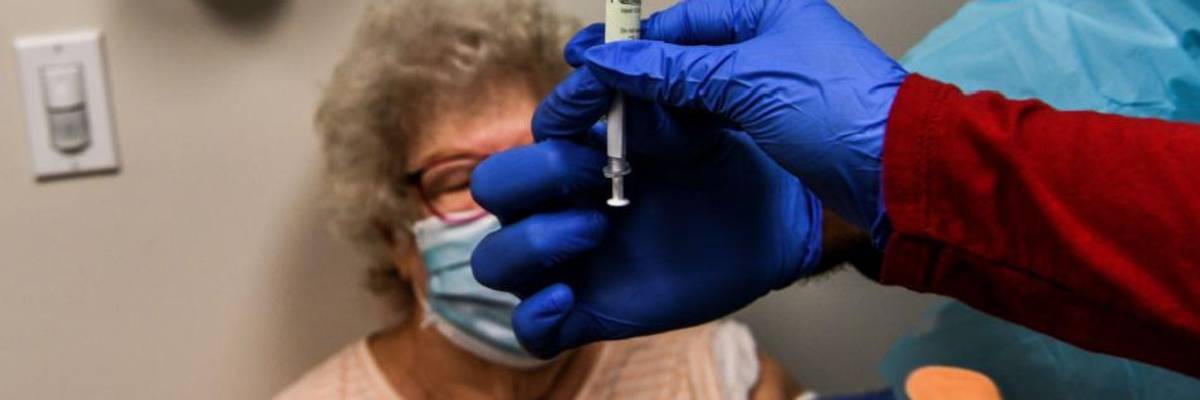
Daisie Esseie, a medic, receives a Pfizer-BioNtech Covid-19 vaccine at the Research Centers of America in Hollywood, Florida on December 18, 2020. (Photo: Chandan Khanna/AFP via Getty Images)
Rep. Pramila Jayapal, who authored the Medicare for All Act of 2019 in the House and gathered 118 cosponsors for the legislation, said Friday that new reporting about surprise medical bills associated with coronavirus vaccinations provide the latest evidence that everyone in the U.S. should be covered under the popular, decades-old Medicare program.
As the New York Times reported Thursday, despite several federal rules put in place this year to ensure patients won't be charged for treatments, testing, and vaccines for the coronavirus, millions of Americans may not be protected.
"It is the American healthcare system, so there are bound to be loopholes we can't anticipate right now," Sabrina Corlette, co-director of the Center on Health Insurance Reforms at Georgetown University, told the Times.
Responding to the article, Jayapal (D-Wash.) wrote on social media that coronavirus vaccines like the one developed by Pfizer, which was rolled out this week and has been administered to thousands of frontline healthcare workers, "must be free and available for everyone."
To ensure all patients, during and after the pandemic, can get the care they need without worrying about unexpected costs, Jayapal said, "It's time for Medicare for All."
As Common Dreams reported in March, in the early days of the public health crisis it was already evident that people were being charged exorbitant, unexpected fees when they got government-mandated coronavirus tests. One Pennsylvania man was charged nearly $4,000 after being tested following his evacuation from Wuhan, China.
Even after Congress passed the CARES Act in March, including rules mandating that insurance companies cover all the costs of coronavirus tests--even if they are administered by out-of-network providers--insurers have still hit patients with bills for thousands of dollars, likely preventing many from pursuing testing and treatment and putting public health at greater risk.
The CARES Act required insurance companies to fully cover federally recommended preventative care within 15 days of recommendations being released, strengthening existing protections under the Affordable Care Act (ACA). The CDC has also barred vaccine providers from billing patients for the vaccine, with out-of-network doctors facing caps of $16.94 for the first dose and $28.39 for the second.
But as the Times reported, millions of Americans are covered by insurance companies that are exempt from the ACA's rules. Those companies could charge administrative fees, holding patients accountable for "visit fees" which some providers charge for all in-person visits, or "facility fees."
For 28.9 million uninsured Americans, there are no rules in place to make sure their vaccinations are covered. As the Times reported:
The United States does not have a national program to cover vaccination costs for them. For coronavirus, it is instructing health providers to submit costs associated with vaccination to a $175 billion Provider Relief Fund created last spring. The fund had $30 billion remaining as of November 10. There's no backup source of funding for the uninsured to get covered if it's depleted.
"Millions of uninsured people could fall through the cracks," tweeted TalkPoverty.org, part of the Center for American Progress.
The Times report came as a bipartisan group of 27 senators urged leaders on Capitol Hill to include protections from surprise medical bills in the spending package lawmakers are currently negotiating.
The American Medical Association is opposed to the inclusion, saying physicians who work at small practices would not receive "fair compensation" for services provided, under the arbitration process that the bill would put in place between insurers and providers. According to the Washington Post, "The arbiters would be guided by the median in-network rates for the services covered, which resembles the price-benchmarking approach that consumer advocates favored."
The Coalition Against Surprise Medical Billing also voiced its opposition to the proposal's approach this week, saying it will mainly benefit private equity firms which own large medical practices.
"Arbitration is not a solution to the surprise billing crisis. It's a gift to private equity firms that have pushed arbitration from the very beginning in order to preserve their business model at the expense of American consumers," the coalition said. "Worse, arbitration erodes the fundamental consumer protections that keep patients' premiums stable. Our members strongly oppose arbitration in any form and urge policymakers not to move forward with this egregious policy."
On social media, the coalition wrote on Friday that "Congress should prioritize reforms that stop these charges and lower costs for families and workers."
According to the Post, despite disagreements over the details of the bill, "The measure mostly protects patients from surprise medical bills."
"For the first time, physicians and facilities couldn't charge patients for the difference between in-network cost sharing and total charges, in what's called balance billing," the Post reported Friday. "The prohibition would apply to emergency medical services at out-of-network facilities and out-of-network providers at in-network hospitals. It would also apply to air ambulances, who were left out of previous iterations of the legislation."
Dear Common Dreams reader, It’s been nearly 30 years since I co-founded Common Dreams with my late wife, Lina Newhouser. We had the radical notion that journalism should serve the public good, not corporate profits. It was clear to us from the outset what it would take to build such a project. No paid advertisements. No corporate sponsors. No millionaire publisher telling us what to think or do. Many people said we wouldn't last a year, but we proved those doubters wrong. Together with a tremendous team of journalists and dedicated staff, we built an independent media outlet free from the constraints of profits and corporate control. Our mission has always been simple: To inform. To inspire. To ignite change for the common good. Building Common Dreams was not easy. Our survival was never guaranteed. When you take on the most powerful forces—Wall Street greed, fossil fuel industry destruction, Big Tech lobbyists, and uber-rich oligarchs who have spent billions upon billions rigging the economy and democracy in their favor—the only bulwark you have is supporters who believe in your work. But here’s the urgent message from me today. It's never been this bad out there. And it's never been this hard to keep us going. At the very moment Common Dreams is most needed, the threats we face are intensifying. We need your support now more than ever. We don't accept corporate advertising and never will. We don't have a paywall because we don't think people should be blocked from critical news based on their ability to pay. Everything we do is funded by the donations of readers like you. When everyone does the little they can afford, we are strong. But if that support retreats or dries up, so do we. Will you donate now to make sure Common Dreams not only survives but thrives? —Craig Brown, Co-founder |
Rep. Pramila Jayapal, who authored the Medicare for All Act of 2019 in the House and gathered 118 cosponsors for the legislation, said Friday that new reporting about surprise medical bills associated with coronavirus vaccinations provide the latest evidence that everyone in the U.S. should be covered under the popular, decades-old Medicare program.
As the New York Times reported Thursday, despite several federal rules put in place this year to ensure patients won't be charged for treatments, testing, and vaccines for the coronavirus, millions of Americans may not be protected.
"It is the American healthcare system, so there are bound to be loopholes we can't anticipate right now," Sabrina Corlette, co-director of the Center on Health Insurance Reforms at Georgetown University, told the Times.
Responding to the article, Jayapal (D-Wash.) wrote on social media that coronavirus vaccines like the one developed by Pfizer, which was rolled out this week and has been administered to thousands of frontline healthcare workers, "must be free and available for everyone."
To ensure all patients, during and after the pandemic, can get the care they need without worrying about unexpected costs, Jayapal said, "It's time for Medicare for All."
As Common Dreams reported in March, in the early days of the public health crisis it was already evident that people were being charged exorbitant, unexpected fees when they got government-mandated coronavirus tests. One Pennsylvania man was charged nearly $4,000 after being tested following his evacuation from Wuhan, China.
Even after Congress passed the CARES Act in March, including rules mandating that insurance companies cover all the costs of coronavirus tests--even if they are administered by out-of-network providers--insurers have still hit patients with bills for thousands of dollars, likely preventing many from pursuing testing and treatment and putting public health at greater risk.
The CARES Act required insurance companies to fully cover federally recommended preventative care within 15 days of recommendations being released, strengthening existing protections under the Affordable Care Act (ACA). The CDC has also barred vaccine providers from billing patients for the vaccine, with out-of-network doctors facing caps of $16.94 for the first dose and $28.39 for the second.
But as the Times reported, millions of Americans are covered by insurance companies that are exempt from the ACA's rules. Those companies could charge administrative fees, holding patients accountable for "visit fees" which some providers charge for all in-person visits, or "facility fees."
For 28.9 million uninsured Americans, there are no rules in place to make sure their vaccinations are covered. As the Times reported:
The United States does not have a national program to cover vaccination costs for them. For coronavirus, it is instructing health providers to submit costs associated with vaccination to a $175 billion Provider Relief Fund created last spring. The fund had $30 billion remaining as of November 10. There's no backup source of funding for the uninsured to get covered if it's depleted.
"Millions of uninsured people could fall through the cracks," tweeted TalkPoverty.org, part of the Center for American Progress.
The Times report came as a bipartisan group of 27 senators urged leaders on Capitol Hill to include protections from surprise medical bills in the spending package lawmakers are currently negotiating.
The American Medical Association is opposed to the inclusion, saying physicians who work at small practices would not receive "fair compensation" for services provided, under the arbitration process that the bill would put in place between insurers and providers. According to the Washington Post, "The arbiters would be guided by the median in-network rates for the services covered, which resembles the price-benchmarking approach that consumer advocates favored."
The Coalition Against Surprise Medical Billing also voiced its opposition to the proposal's approach this week, saying it will mainly benefit private equity firms which own large medical practices.
"Arbitration is not a solution to the surprise billing crisis. It's a gift to private equity firms that have pushed arbitration from the very beginning in order to preserve their business model at the expense of American consumers," the coalition said. "Worse, arbitration erodes the fundamental consumer protections that keep patients' premiums stable. Our members strongly oppose arbitration in any form and urge policymakers not to move forward with this egregious policy."
On social media, the coalition wrote on Friday that "Congress should prioritize reforms that stop these charges and lower costs for families and workers."
According to the Post, despite disagreements over the details of the bill, "The measure mostly protects patients from surprise medical bills."
"For the first time, physicians and facilities couldn't charge patients for the difference between in-network cost sharing and total charges, in what's called balance billing," the Post reported Friday. "The prohibition would apply to emergency medical services at out-of-network facilities and out-of-network providers at in-network hospitals. It would also apply to air ambulances, who were left out of previous iterations of the legislation."
Rep. Pramila Jayapal, who authored the Medicare for All Act of 2019 in the House and gathered 118 cosponsors for the legislation, said Friday that new reporting about surprise medical bills associated with coronavirus vaccinations provide the latest evidence that everyone in the U.S. should be covered under the popular, decades-old Medicare program.
As the New York Times reported Thursday, despite several federal rules put in place this year to ensure patients won't be charged for treatments, testing, and vaccines for the coronavirus, millions of Americans may not be protected.
"It is the American healthcare system, so there are bound to be loopholes we can't anticipate right now," Sabrina Corlette, co-director of the Center on Health Insurance Reforms at Georgetown University, told the Times.
Responding to the article, Jayapal (D-Wash.) wrote on social media that coronavirus vaccines like the one developed by Pfizer, which was rolled out this week and has been administered to thousands of frontline healthcare workers, "must be free and available for everyone."
To ensure all patients, during and after the pandemic, can get the care they need without worrying about unexpected costs, Jayapal said, "It's time for Medicare for All."
As Common Dreams reported in March, in the early days of the public health crisis it was already evident that people were being charged exorbitant, unexpected fees when they got government-mandated coronavirus tests. One Pennsylvania man was charged nearly $4,000 after being tested following his evacuation from Wuhan, China.
Even after Congress passed the CARES Act in March, including rules mandating that insurance companies cover all the costs of coronavirus tests--even if they are administered by out-of-network providers--insurers have still hit patients with bills for thousands of dollars, likely preventing many from pursuing testing and treatment and putting public health at greater risk.
The CARES Act required insurance companies to fully cover federally recommended preventative care within 15 days of recommendations being released, strengthening existing protections under the Affordable Care Act (ACA). The CDC has also barred vaccine providers from billing patients for the vaccine, with out-of-network doctors facing caps of $16.94 for the first dose and $28.39 for the second.
But as the Times reported, millions of Americans are covered by insurance companies that are exempt from the ACA's rules. Those companies could charge administrative fees, holding patients accountable for "visit fees" which some providers charge for all in-person visits, or "facility fees."
For 28.9 million uninsured Americans, there are no rules in place to make sure their vaccinations are covered. As the Times reported:
The United States does not have a national program to cover vaccination costs for them. For coronavirus, it is instructing health providers to submit costs associated with vaccination to a $175 billion Provider Relief Fund created last spring. The fund had $30 billion remaining as of November 10. There's no backup source of funding for the uninsured to get covered if it's depleted.
"Millions of uninsured people could fall through the cracks," tweeted TalkPoverty.org, part of the Center for American Progress.
The Times report came as a bipartisan group of 27 senators urged leaders on Capitol Hill to include protections from surprise medical bills in the spending package lawmakers are currently negotiating.
The American Medical Association is opposed to the inclusion, saying physicians who work at small practices would not receive "fair compensation" for services provided, under the arbitration process that the bill would put in place between insurers and providers. According to the Washington Post, "The arbiters would be guided by the median in-network rates for the services covered, which resembles the price-benchmarking approach that consumer advocates favored."
The Coalition Against Surprise Medical Billing also voiced its opposition to the proposal's approach this week, saying it will mainly benefit private equity firms which own large medical practices.
"Arbitration is not a solution to the surprise billing crisis. It's a gift to private equity firms that have pushed arbitration from the very beginning in order to preserve their business model at the expense of American consumers," the coalition said. "Worse, arbitration erodes the fundamental consumer protections that keep patients' premiums stable. Our members strongly oppose arbitration in any form and urge policymakers not to move forward with this egregious policy."
On social media, the coalition wrote on Friday that "Congress should prioritize reforms that stop these charges and lower costs for families and workers."
According to the Post, despite disagreements over the details of the bill, "The measure mostly protects patients from surprise medical bills."
"For the first time, physicians and facilities couldn't charge patients for the difference between in-network cost sharing and total charges, in what's called balance billing," the Post reported Friday. "The prohibition would apply to emergency medical services at out-of-network facilities and out-of-network providers at in-network hospitals. It would also apply to air ambulances, who were left out of previous iterations of the legislation."