

SUBSCRIBE TO OUR FREE NEWSLETTER
Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
5
#000000
#FFFFFF
To donate by check, phone, or other method, see our More Ways to Give page.


Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
In 1998, Dr. Deb Richter began, almost single handedly, to revive the dream of universal health care in the United States--open to all and paid for by the government. A primary care physician from Buffalo, New York, Richter had become outraged by the barriers to accessing quality health care in the city's low-income communities.
In 1998, Dr. Deb Richter began, almost single handedly, to revive the dream of universal health care in the United States--open to all and paid for by the government. A primary care physician from Buffalo, New York, Richter had become outraged by the barriers to accessing quality health care in the city's low-income communities.
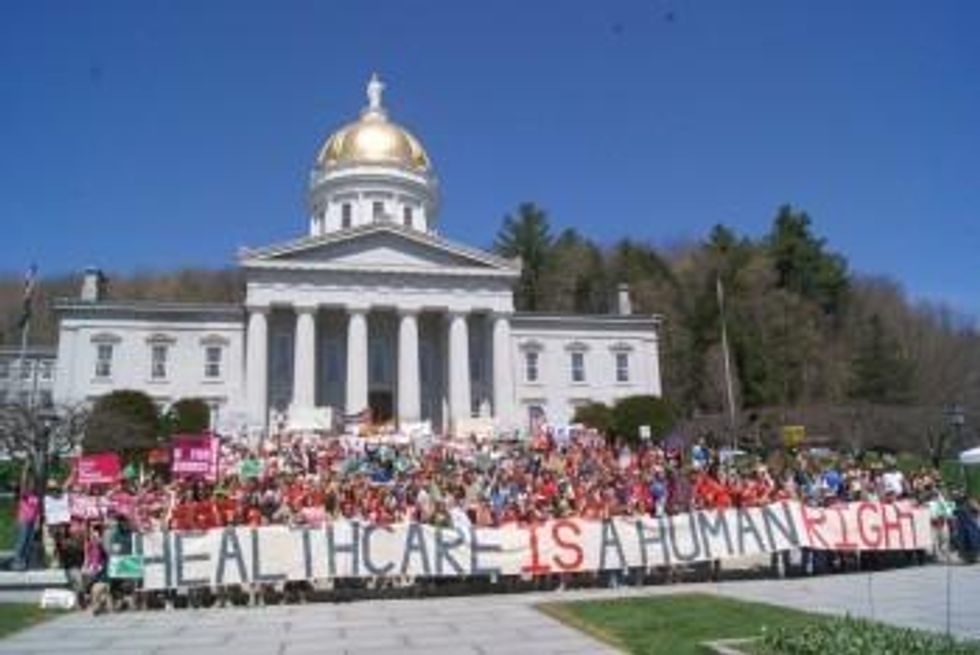
The existing system of privatized health care was expensive, opaque, and unfair, and yet reforming health care--as President Obama has discovered--means taking on a multi-billion dollar insurance industry that vociferously lobbies to maintain its profits.
Despairing of ever advancing universal care in the state of New York, Dr. Richter moved to Vermont where she thought that politics were on a scale where she could have an impact. Practicing medicine three days a week, Dr. Richter used the rest of her time to travel the state speaking about a so-called single payer system that would dispose of the multitude of private insurance companies and offer patients a simple point-of-access health care. Recognizing that businesses and doctors were key constituencies, she spoke to every Rotary Club and every business association that would have her, as well as to any doctor who would listen. She also started a new organization devoted solely to educating the public about the single payer system. She helped organize a rally that drew 1,000 people to the state capital. Eventually, Dr. Richter found her way inside the statehouse, where she formed alliances with legislators from all three parties--Democrat, Republican, and Progressive.
In 2011, with Dr. Richter standing by the Governor's side as he signed the bill, Vermont became the first state to enact a framework and a timetable for a state-level single payer health system. Implementation of the law now waits for the clearance of a number of crucial hurdles, among them a federal waiver of requirements in the Patient Protection and Affordable Care Act--Obamacare--and the passage of a financing plan that would raise enough new tax revenue to replace what is currently spent on private health insurance premiums.
Obamacare has been criticized by both the left and right for its failure to simplify the system or curb costs. There is a certain irony in the fact that President Obama's reforms-- which left the private insurance industry untouched and failed to introduce a "public option" that would force private insurers to lower their prices--might derail the Vermont initiative, which is designed to do both. Vermont's single payer plan would eliminate the private health care exchanges in which the uninsured will be mandated to buy insurance or pay a fine under Obamacare. Instead, Vermont would provide publicly funded health care for all residents. Federal law dictates that in order to do this, Vermont must obtain a waiver from the U.S. Secretary of Health and Human Services sanctioning the state initiative, thus enabling Vermont to continue receiving the federal dollars that would have subsidized the exchange. That remains a hurdle, but the state legislators shaping the bill are confident they will get the waiver.
Financing the single payer system is the other challenge. Vermont's lawmakers have until 2017--when the reforms come in effect--to raise $1.6 billion in new taxes to replace private insurance premiums and to cover the health care costs of those who are now uninsured. That presents a formidable challenge for a cash-strapped rural economy. Vermont already has some of the highest taxes in the country, although it has weathered the financial crisis more successfully than its southern neighbors by avoiding a housing bubble. New taxes might mean a 1 percent assessment on individuals' gross incomes and a 6--8.5 percent payroll tax. Local polling suggests that Vermonters are happy to pay more, provided additional revenue is ringfenced for health care.
The challenges are steep, but Vermont stands on the verge of a historic change--one that would make it the first U.S. state to have a universal health care system that is comparable with other developed countries. Could this be a tipping point in the battle against America epic health care problems? Could it also be the story of how an impassioned few succeeded in transforming their community?

Chris Wood, one of the original activists, said he was drawn to the concept of single payer because it was based on the premise that health care is a public good, comparable to public schools and fire departments. "It didn't make much sense to me," said Wood, "that something as important as health care should be left to the marketplace, where your wealth or your income might determine the kind of care you [are] able to get."
Wood and the other activists realized that neither the "crisis" nor its perceived solution were new. Norway has had a single payer health care system since 1912; Japan has had one since 1938. The United Kingdom began its single payer in 1948; Canada implemented one in 1966; and Taiwan did so in 1995. While all these countries pay for health care from a single government fund, the delivery system varies from country to country. In the U.K., the government not only finances health care, it also provides it through a national health service. On the other hand, Canada's single payer financing is funneled to private sector hospitals and physicians.
The total number of single payer countries around the world is hard to estimate because the term is not uniformly defined. Using the purest definition, only about 20 countries are truly single payer, the vast majority in the developed world. However, there are scores of countries, such as France and the Netherlands, which use a single payer to finance a basic benefit package for all citizens while allowing private or employment-based financing to cover additional services. Other countries, such as Switzerland and Germany, are generally thought to have multi-payer systems because they rely heavily on employment-based "sickness funds." However, the sickness funds are almost instrumentalities of the government because they are so tightly regulated and therefore bear little resemblance to for-profit U.S. insurance companies. Thus, among developed countries, only the U.S. fails to use the power of government to ensure health care access for all of its people. At the same time, the U.S. is the biggest spender on health care.
Although the U.S. made an important step toward universal care in 1965 with the enactment of Medicare and Medicaid, Obamacare is the only significant reform to have happened since, and many expect that Obamacare will fall short of providing universal access and controlling costs. Medicare, on the other hand, has been relatively successful in holding down costs. It pays providers according to a fixed fee schedule, and incurs administrative expenses of only 3.1 percent, compared to an average of 14.1 percent for private insurance, according to a 2005 study by the American Medical Association. But Medicare leaves out everyone under age 65 and Medicaid only covers the very poor. By the 1970s, many people who were not eligible for either federal program were finding that health care expenses, even with insurance, put them at serious financial risk.
In 1972, Senator Edward Kennedy authored the book In Critical Condition: The Crisis in America's Health Care. The book was based on the testimony of people Kennedy had invited to speak at Senate subcommittee hearings. Witnesses told of becoming pauperized from medical debt. They spoke of the unaffordability of health insurance, and decried the indignity of charity care. They chronicled the difficulty of finding doctors in low-income neighborhoods, and of navigating the confusing maze of services and insurance coverage. Others testified that they had trouble receiving good care, that the health care industry was profit-oriented and monopolistic, and that they had no say in the quality or availability of health care services.
Kennedy contrasted U.S. health care with what he had seen in trips to Sweden, Denmark, Norway, and Israel, and with what he had learned about the United Kingdom. "Most of us have been led to believe that health care is a disaster in Europe," he wrote. "From what I saw, these things are simply false. The fact is, while most Americans are angry and frustrated about health care, most Englishmen, Danes, Swedes, and Israelis are not." Kennedy concluded his book by calling for a program in which "the federal government would become the health insurance carrier for the entire nation." Kennedy was proposing a single payer system, although he did not use that term.

In 1988, 10 percent of Vermonters had no health insurance; thousands more were underinsured. Farmers, loggers, artists, or convenience store owners who got seriously ill often faced financial ruin. The access crisis--a plight shared by other U.S. states--was compounded by health care costs that were rising at greater than the inflation rate. Employers and individuals often saw double digit annual increases in insurance premiums, and those without insurance who attempted to pay hospital bills out of pocket paid the highest rates of all. The health care system was also rife with excessive administrative costs related to its fragmented financing streams. Providers had to deal with scores of payers--insurance companies, multiple insurance policies, federal and state health plans, and private individuals. The insurance industry in particular added immense cost to the system without adding anything of value in terms of health care. Furthermore, the fragmentation of financing meant that payers had little bargaining power in purchasing pharmaceuticals or medical equipment, nor any say in hospital spending. As costs kept escalating, any attempt to curtail spending in one area simply caused an increase in charges somewhere else.
However, because the U.S. Congress showed no inclination to consider reforms resembling the universal health care systems in other developed countries, the health care activists in Vermont concluded that state-level initiatives were the only hope. The activists told themselves that the momentum for reform builds over time, but when the time is ripe, change happens with surprising speed. The important thing was to have thought through the solution and to have educated the public about its merits, so that when the opportune moment arrived, a reorganized health care system would reveal itself as the most practical response.
In 1989, they established a small nonprofit called the Vermont Consumers' Campaign for Health. They raised funds, hired staff, and built a citizens' movement. They sponsored educational forums around the state, published a newsletter, and arranged meetings with labor unions, consumer groups, businesses, teachers, town officials, and politicians. The organization coordinated referenda on single payer health care at more than 50 town meetings, and drummed up support for a single payer bill to be introduced in the Vermont legislature.
The response to the group's efforts was overwhelmingly positive. Vermonters readily accepted the notion that the state should be everyone's health insurer. Businesses would be relieved of the burden of buying health insurance for employees. Labor unions would no longer have to fight for health benefits at every contract negotiation. All Vermonters would share in financing the program, and therefore all Vermonters would have a stake in ensuring its quality and efficiency.
However, the populace was ahead of its elected officials on the issue. Although single payer advocates had a big ally in Vermont's Independent former-Congressman Bernie Sanders, who had been busy in Washington trying to advance a national single payer proposal, Sanders' enthusiasm was not shared by state legislators. The health care committee chairpersons felt that other matters were more pressing and less politically charged. Thus, the first single payer bill to be introduced in the legislature (in 1991) never even got a committee hearing. The following year, former-Governor Howard Dean, himself a physician, failed to back the proposals, perhaps with an eye to his later presidential bid that was well-funded by the insurance industry.
The mid-90s saw increased focus on health care at the national level. The Clinton administration was promoting health reform based on "managed competition" among private insurers. Ultimately the effort was easily defeated by Congress. Meanwhile, in Vermont, a tiny minority of Progressive Party lawmakers finally succeeded in forcing a vote on the single payer system, but fell short. Instead, the idea of "managed care" was adopted in Vermont and elsewhere, a system that saved money for a year or two before simply becoming a vehicle for denying care and increasing insurance company profits. Consumers reacted by demanding a return to more traditional insurance policies.
The single payer movement might have died then and there, if not for the campaigning of Dr. Richter at the turn of the millennium. The need to corral costs had never been so urgent. Vermont's overall health care expenditures had doubled in less than 10 years. Health care had become a $5 billion per year industry in Vermont--19 percent of the gross domestic product. Yet, Vermont's governor at the time--Republican Jim Douglas--continued to oppose reform, even though a new state-commissioned study in 2001 showed that single payer would save $118 million annually, roughly a 5 percent reduction in Vermont's total health care spending.
It wasn't until 2010 that State Senator Peter Shumlin, also a gubernatorial candidate, dared to make the single payer system a centerpiece of his primary campaign. Shumlin had voted for the earlier single payer proposal, and had helped the legislature appropriate money for a Harvard professor, William Hsiao, to design an exhaustive study of how a universal health care system in Vermont might work.
Shumlin faced an uphill battle as polls showed him trailing his competitors early in the primary season. That's when Dr. Richter and a Middlebury College professor, Ellen Oxfeld, kicked into action--day after day on the phone, sending emails, attending meetings, pleading with friends and colleagues to support the single payer candidate. If Shumlin won, they said, Vermont would have a chance to lead the nation toward universal health care, just as Saskatchewan had led Canada to single payer decades before. People listened--and voted. Shumlin narrowly won the nomination, then went on to defeat his Republican opponent in the general election.
"The grassroots support I got from single payer advocates made it possible for me to be governor," Shumlin told an interviewer from Vermont Life magazine. "They knocked on doors. They poured their hearts out. They saw an opportunity and I would not be here without them."
As Shumlin took office, Professor Hsiao issued his report containing designs of three models that built on the state's previous reform efforts: a government-run single payer, a public option, and a public-private single payer that preserved some role for insurance companies in administering claims. It was this third option that was chosen, based on its eye-catch savings of 25 percent over the next decade. Hsiao attributed these savings to administrative simplification, reductions in fraud and abuse, reformed payment systems for doctors and hospitals, and no-fault medical malpractice reform.
Passage of a single payer bill was far from a sure thing, despite a democrat-controlled legislature. The major private health insurer in the state, Blue Cross Blue Shield, annually spends more on lobbying the state legislature than almost any other private firm. The pharmaceutical industry and the hospital association are not far behind. But with a population of only 600,000, Vermont's legislative process is so intimate that the voices of private citizens can sometimes have impact equal to the professional lobbyists. A cascade of concerned citizens flooded the statehouse in favor of single payer. Most visible were members of a "Health Care is a Human Right" campaign organized by the pro-labor Vermont Workers' Center. Wearing red t-shirts, they filled the committee rooms and visitors' galleries, watching every debate, and reading every mark-up of the bill. Dr. Richter's group was also present and single payer supporters throughout the state were kept up-to-date by email.
The bill that passed and was signed into law in the spring of 2011 laid the foundation for Green Mountain Care, the purpose of which was "to provide, as a public good, comprehensive, affordable, high quality, publicly financed health care coverage for all Vermont residents in a seamless and equitable manner regardless of income, assets, health status, or availability of other coverage." The law established a five-member board to oversee the program and administer payments to providers from a dedicated fund. The program would contain costs by reducing unnecessary administrative expenses and establishing innovative payment mechanisms to providers, such as global budgets to hospitals.
However, the law left several items of business unfinished. First was the uncertain interface with Obamacare, the federal health care law passed by Congress the previous fall. National health care reform was clearly headed in a different direction from Vermont's single payer system. Obamacare will require all individuals to have insurance by 2014. Those not covered by Medicare or Medicaid must purchase private insurance in health care "exchanges." Federal subsidies will be available to individuals who qualify on the basis of income. No state may proceed in a different manner unless granted a federal waiver, and Obamacare explicitly prohibits waivers until 2017 at the earliest. That means that implementation of Green Mountain Care will have to wait.
Second, the Vermont law did not include a benefits package or a financing plan. The omission of a financing plan has drawn controversy, with critics charging that the Shumlin administration wants to avoid talking about what may be the largest tax increase in Vermont history. What the naysayers fail to mention, however, is that taxes would replace private insurance premiums and, by most estimates, Green Mountain Care would cover everyone for less total dollars than are currently spent in a system that leaves many uninsured.
The financing question has not been totally ignored. To fulfill a requirement of the new law, the Shumlin administration asked analysts at the University of Massachusetts to formulate baseline data for financing Green Mountain Care and to examine the financial implications of a federal health care exchange. The UMass report once again confirmed that a state single payer could cover everyone and still save money over the spending projections absent reform, but it stopped short of naming specific revenue sources, which was what single payer opponents had been clamoring for so that they could raise a hue and cry about taxes. Shumlin countered by pointing out that Green Mountain Care could not begin offering health coverage until 2017 at the earliest because of the Obamacare preemption, and therefore, he argued, a financing proposal would be premature.
Critics have also cried that doctors will leave the state when Green Mountain Care is implemented. Yet, while one or two specialists have indicated they might seek greener pastures elsewhere, there have been at least as many doctors outside the state who have said they would consider moving to Vermont so they could practice under a single payer system, and not have to worry about multiple insurance companies and whether their patients could afford needed care.
Vermont's efforts contain lessons for other states looking at enacting universal health care. The first lesson is that the design of a state-level system can be more complex than the design might be for a federal Medicare-for-all plan. For one thing, a state-level single payer must wrap around existing federal programs such as Medicare and Medicaid, or obtain waivers to capture the federal funds and apply them to the state plan. In addition, there are many cross-border issues that uniquely burden state-level initiatives. For instance, residents of one state may obtain health care services in another state. Others may live in one state but work in another. The question then becomes how to negotiate and pay for out-of-state services and how to adjust tax exposure for residents who may have out-of-state insurance. Finally, there is the question of the Employee Retirement Income Security Act (ERISA), the federal law that allows large employers to self-insure. ERISA prohibits states from interfering in self-insure health plans, but would probably not preclude a state payroll tax on all employers to support a universal health care plan. This would leave ERISA employers with the decision of whether to drop their self-insurance or try to challenge the payroll tax in federal court. No one, not even Hsiao, has been able to predict the outcome of a legal challenge to single payer financing based on the ERISA law. It remains one of the unknowns for Vermont going forward.
Vermont's single payer supporters have caught their breath, but have not exactly relaxed their efforts in advocating for the ultimate goal. The implementation of Obamacare in 2014 will be closely watched, as will the state's roll-out of the single payer benefits package and financing plan. Well-funded attacks on the Vermont single payer initiative have already been launched by political action committees and by Governor Shumlin's political opponents. These attacks play on the public's fear of change. But Vermonters are independent thinkers, and the single payer advocates have been quickly responding to the naysayers with letters to the editor and press releases reiterating the well-researched projections showing that single payer will save money.
The grand vision of Green Mountain Care continues to hold great promise: To treat all human beings as equals when it comes to necessary health care; to end the absurd spiral of health care costs that is crippling businesses, bankrupting school and municipal budgets, and threatening the entire economy; and to give doctors the ability to practice the kind of medicine for which they were trained--focusing on patients' needs, not on billing, insurance, and a patients' financial status. A majority of Vermonters are cautiously optimistic that, in four years, their state will become the first place in America to realize this dream.
Dear Common Dreams reader, The U.S. is on a fast track to authoritarianism like nothing I've ever seen. Meanwhile, corporate news outlets are utterly capitulating to Trump, twisting their coverage to avoid drawing his ire while lining up to stuff cash in his pockets. That's why I believe that Common Dreams is doing the best and most consequential reporting that we've ever done. Our small but mighty team is a progressive reporting powerhouse, covering the news every day that the corporate media never will. Our mission has always been simple: To inform. To inspire. And to ignite change for the common good. Now here's the key piece that I want all our readers to understand: None of this would be possible without your financial support. That's not just some fundraising cliche. It's the absolute and literal truth. We don't accept corporate advertising and never will. We don't have a paywall because we don't think people should be blocked from critical news based on their ability to pay. Everything we do is funded by the donations of readers like you. Will you donate now to help power the nonprofit, independent reporting of Common Dreams? Thank you for being a vital member of our community. Together, we can keep independent journalism alive when it’s needed most. - Craig Brown, Co-founder |
In 1998, Dr. Deb Richter began, almost single handedly, to revive the dream of universal health care in the United States--open to all and paid for by the government. A primary care physician from Buffalo, New York, Richter had become outraged by the barriers to accessing quality health care in the city's low-income communities.
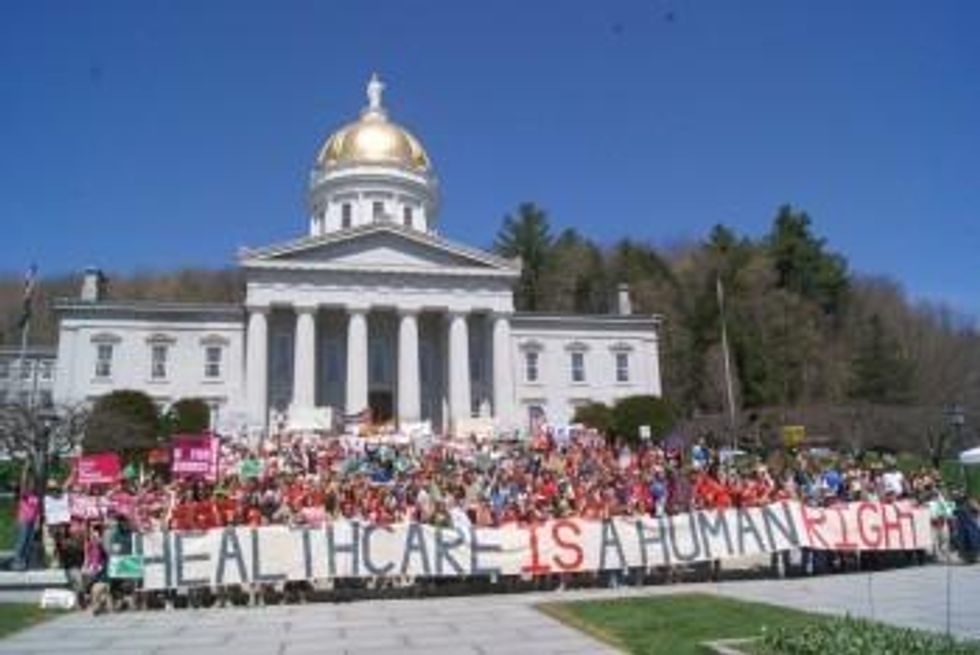
The existing system of privatized health care was expensive, opaque, and unfair, and yet reforming health care--as President Obama has discovered--means taking on a multi-billion dollar insurance industry that vociferously lobbies to maintain its profits.
Despairing of ever advancing universal care in the state of New York, Dr. Richter moved to Vermont where she thought that politics were on a scale where she could have an impact. Practicing medicine three days a week, Dr. Richter used the rest of her time to travel the state speaking about a so-called single payer system that would dispose of the multitude of private insurance companies and offer patients a simple point-of-access health care. Recognizing that businesses and doctors were key constituencies, she spoke to every Rotary Club and every business association that would have her, as well as to any doctor who would listen. She also started a new organization devoted solely to educating the public about the single payer system. She helped organize a rally that drew 1,000 people to the state capital. Eventually, Dr. Richter found her way inside the statehouse, where she formed alliances with legislators from all three parties--Democrat, Republican, and Progressive.
In 2011, with Dr. Richter standing by the Governor's side as he signed the bill, Vermont became the first state to enact a framework and a timetable for a state-level single payer health system. Implementation of the law now waits for the clearance of a number of crucial hurdles, among them a federal waiver of requirements in the Patient Protection and Affordable Care Act--Obamacare--and the passage of a financing plan that would raise enough new tax revenue to replace what is currently spent on private health insurance premiums.
Obamacare has been criticized by both the left and right for its failure to simplify the system or curb costs. There is a certain irony in the fact that President Obama's reforms-- which left the private insurance industry untouched and failed to introduce a "public option" that would force private insurers to lower their prices--might derail the Vermont initiative, which is designed to do both. Vermont's single payer plan would eliminate the private health care exchanges in which the uninsured will be mandated to buy insurance or pay a fine under Obamacare. Instead, Vermont would provide publicly funded health care for all residents. Federal law dictates that in order to do this, Vermont must obtain a waiver from the U.S. Secretary of Health and Human Services sanctioning the state initiative, thus enabling Vermont to continue receiving the federal dollars that would have subsidized the exchange. That remains a hurdle, but the state legislators shaping the bill are confident they will get the waiver.
Financing the single payer system is the other challenge. Vermont's lawmakers have until 2017--when the reforms come in effect--to raise $1.6 billion in new taxes to replace private insurance premiums and to cover the health care costs of those who are now uninsured. That presents a formidable challenge for a cash-strapped rural economy. Vermont already has some of the highest taxes in the country, although it has weathered the financial crisis more successfully than its southern neighbors by avoiding a housing bubble. New taxes might mean a 1 percent assessment on individuals' gross incomes and a 6--8.5 percent payroll tax. Local polling suggests that Vermonters are happy to pay more, provided additional revenue is ringfenced for health care.
The challenges are steep, but Vermont stands on the verge of a historic change--one that would make it the first U.S. state to have a universal health care system that is comparable with other developed countries. Could this be a tipping point in the battle against America epic health care problems? Could it also be the story of how an impassioned few succeeded in transforming their community?

Chris Wood, one of the original activists, said he was drawn to the concept of single payer because it was based on the premise that health care is a public good, comparable to public schools and fire departments. "It didn't make much sense to me," said Wood, "that something as important as health care should be left to the marketplace, where your wealth or your income might determine the kind of care you [are] able to get."
Wood and the other activists realized that neither the "crisis" nor its perceived solution were new. Norway has had a single payer health care system since 1912; Japan has had one since 1938. The United Kingdom began its single payer in 1948; Canada implemented one in 1966; and Taiwan did so in 1995. While all these countries pay for health care from a single government fund, the delivery system varies from country to country. In the U.K., the government not only finances health care, it also provides it through a national health service. On the other hand, Canada's single payer financing is funneled to private sector hospitals and physicians.
The total number of single payer countries around the world is hard to estimate because the term is not uniformly defined. Using the purest definition, only about 20 countries are truly single payer, the vast majority in the developed world. However, there are scores of countries, such as France and the Netherlands, which use a single payer to finance a basic benefit package for all citizens while allowing private or employment-based financing to cover additional services. Other countries, such as Switzerland and Germany, are generally thought to have multi-payer systems because they rely heavily on employment-based "sickness funds." However, the sickness funds are almost instrumentalities of the government because they are so tightly regulated and therefore bear little resemblance to for-profit U.S. insurance companies. Thus, among developed countries, only the U.S. fails to use the power of government to ensure health care access for all of its people. At the same time, the U.S. is the biggest spender on health care.
Although the U.S. made an important step toward universal care in 1965 with the enactment of Medicare and Medicaid, Obamacare is the only significant reform to have happened since, and many expect that Obamacare will fall short of providing universal access and controlling costs. Medicare, on the other hand, has been relatively successful in holding down costs. It pays providers according to a fixed fee schedule, and incurs administrative expenses of only 3.1 percent, compared to an average of 14.1 percent for private insurance, according to a 2005 study by the American Medical Association. But Medicare leaves out everyone under age 65 and Medicaid only covers the very poor. By the 1970s, many people who were not eligible for either federal program were finding that health care expenses, even with insurance, put them at serious financial risk.
In 1972, Senator Edward Kennedy authored the book In Critical Condition: The Crisis in America's Health Care. The book was based on the testimony of people Kennedy had invited to speak at Senate subcommittee hearings. Witnesses told of becoming pauperized from medical debt. They spoke of the unaffordability of health insurance, and decried the indignity of charity care. They chronicled the difficulty of finding doctors in low-income neighborhoods, and of navigating the confusing maze of services and insurance coverage. Others testified that they had trouble receiving good care, that the health care industry was profit-oriented and monopolistic, and that they had no say in the quality or availability of health care services.
Kennedy contrasted U.S. health care with what he had seen in trips to Sweden, Denmark, Norway, and Israel, and with what he had learned about the United Kingdom. "Most of us have been led to believe that health care is a disaster in Europe," he wrote. "From what I saw, these things are simply false. The fact is, while most Americans are angry and frustrated about health care, most Englishmen, Danes, Swedes, and Israelis are not." Kennedy concluded his book by calling for a program in which "the federal government would become the health insurance carrier for the entire nation." Kennedy was proposing a single payer system, although he did not use that term.

In 1988, 10 percent of Vermonters had no health insurance; thousands more were underinsured. Farmers, loggers, artists, or convenience store owners who got seriously ill often faced financial ruin. The access crisis--a plight shared by other U.S. states--was compounded by health care costs that were rising at greater than the inflation rate. Employers and individuals often saw double digit annual increases in insurance premiums, and those without insurance who attempted to pay hospital bills out of pocket paid the highest rates of all. The health care system was also rife with excessive administrative costs related to its fragmented financing streams. Providers had to deal with scores of payers--insurance companies, multiple insurance policies, federal and state health plans, and private individuals. The insurance industry in particular added immense cost to the system without adding anything of value in terms of health care. Furthermore, the fragmentation of financing meant that payers had little bargaining power in purchasing pharmaceuticals or medical equipment, nor any say in hospital spending. As costs kept escalating, any attempt to curtail spending in one area simply caused an increase in charges somewhere else.
However, because the U.S. Congress showed no inclination to consider reforms resembling the universal health care systems in other developed countries, the health care activists in Vermont concluded that state-level initiatives were the only hope. The activists told themselves that the momentum for reform builds over time, but when the time is ripe, change happens with surprising speed. The important thing was to have thought through the solution and to have educated the public about its merits, so that when the opportune moment arrived, a reorganized health care system would reveal itself as the most practical response.
In 1989, they established a small nonprofit called the Vermont Consumers' Campaign for Health. They raised funds, hired staff, and built a citizens' movement. They sponsored educational forums around the state, published a newsletter, and arranged meetings with labor unions, consumer groups, businesses, teachers, town officials, and politicians. The organization coordinated referenda on single payer health care at more than 50 town meetings, and drummed up support for a single payer bill to be introduced in the Vermont legislature.
The response to the group's efforts was overwhelmingly positive. Vermonters readily accepted the notion that the state should be everyone's health insurer. Businesses would be relieved of the burden of buying health insurance for employees. Labor unions would no longer have to fight for health benefits at every contract negotiation. All Vermonters would share in financing the program, and therefore all Vermonters would have a stake in ensuring its quality and efficiency.
However, the populace was ahead of its elected officials on the issue. Although single payer advocates had a big ally in Vermont's Independent former-Congressman Bernie Sanders, who had been busy in Washington trying to advance a national single payer proposal, Sanders' enthusiasm was not shared by state legislators. The health care committee chairpersons felt that other matters were more pressing and less politically charged. Thus, the first single payer bill to be introduced in the legislature (in 1991) never even got a committee hearing. The following year, former-Governor Howard Dean, himself a physician, failed to back the proposals, perhaps with an eye to his later presidential bid that was well-funded by the insurance industry.
The mid-90s saw increased focus on health care at the national level. The Clinton administration was promoting health reform based on "managed competition" among private insurers. Ultimately the effort was easily defeated by Congress. Meanwhile, in Vermont, a tiny minority of Progressive Party lawmakers finally succeeded in forcing a vote on the single payer system, but fell short. Instead, the idea of "managed care" was adopted in Vermont and elsewhere, a system that saved money for a year or two before simply becoming a vehicle for denying care and increasing insurance company profits. Consumers reacted by demanding a return to more traditional insurance policies.
The single payer movement might have died then and there, if not for the campaigning of Dr. Richter at the turn of the millennium. The need to corral costs had never been so urgent. Vermont's overall health care expenditures had doubled in less than 10 years. Health care had become a $5 billion per year industry in Vermont--19 percent of the gross domestic product. Yet, Vermont's governor at the time--Republican Jim Douglas--continued to oppose reform, even though a new state-commissioned study in 2001 showed that single payer would save $118 million annually, roughly a 5 percent reduction in Vermont's total health care spending.
It wasn't until 2010 that State Senator Peter Shumlin, also a gubernatorial candidate, dared to make the single payer system a centerpiece of his primary campaign. Shumlin had voted for the earlier single payer proposal, and had helped the legislature appropriate money for a Harvard professor, William Hsiao, to design an exhaustive study of how a universal health care system in Vermont might work.
Shumlin faced an uphill battle as polls showed him trailing his competitors early in the primary season. That's when Dr. Richter and a Middlebury College professor, Ellen Oxfeld, kicked into action--day after day on the phone, sending emails, attending meetings, pleading with friends and colleagues to support the single payer candidate. If Shumlin won, they said, Vermont would have a chance to lead the nation toward universal health care, just as Saskatchewan had led Canada to single payer decades before. People listened--and voted. Shumlin narrowly won the nomination, then went on to defeat his Republican opponent in the general election.
"The grassroots support I got from single payer advocates made it possible for me to be governor," Shumlin told an interviewer from Vermont Life magazine. "They knocked on doors. They poured their hearts out. They saw an opportunity and I would not be here without them."
As Shumlin took office, Professor Hsiao issued his report containing designs of three models that built on the state's previous reform efforts: a government-run single payer, a public option, and a public-private single payer that preserved some role for insurance companies in administering claims. It was this third option that was chosen, based on its eye-catch savings of 25 percent over the next decade. Hsiao attributed these savings to administrative simplification, reductions in fraud and abuse, reformed payment systems for doctors and hospitals, and no-fault medical malpractice reform.
Passage of a single payer bill was far from a sure thing, despite a democrat-controlled legislature. The major private health insurer in the state, Blue Cross Blue Shield, annually spends more on lobbying the state legislature than almost any other private firm. The pharmaceutical industry and the hospital association are not far behind. But with a population of only 600,000, Vermont's legislative process is so intimate that the voices of private citizens can sometimes have impact equal to the professional lobbyists. A cascade of concerned citizens flooded the statehouse in favor of single payer. Most visible were members of a "Health Care is a Human Right" campaign organized by the pro-labor Vermont Workers' Center. Wearing red t-shirts, they filled the committee rooms and visitors' galleries, watching every debate, and reading every mark-up of the bill. Dr. Richter's group was also present and single payer supporters throughout the state were kept up-to-date by email.
The bill that passed and was signed into law in the spring of 2011 laid the foundation for Green Mountain Care, the purpose of which was "to provide, as a public good, comprehensive, affordable, high quality, publicly financed health care coverage for all Vermont residents in a seamless and equitable manner regardless of income, assets, health status, or availability of other coverage." The law established a five-member board to oversee the program and administer payments to providers from a dedicated fund. The program would contain costs by reducing unnecessary administrative expenses and establishing innovative payment mechanisms to providers, such as global budgets to hospitals.
However, the law left several items of business unfinished. First was the uncertain interface with Obamacare, the federal health care law passed by Congress the previous fall. National health care reform was clearly headed in a different direction from Vermont's single payer system. Obamacare will require all individuals to have insurance by 2014. Those not covered by Medicare or Medicaid must purchase private insurance in health care "exchanges." Federal subsidies will be available to individuals who qualify on the basis of income. No state may proceed in a different manner unless granted a federal waiver, and Obamacare explicitly prohibits waivers until 2017 at the earliest. That means that implementation of Green Mountain Care will have to wait.
Second, the Vermont law did not include a benefits package or a financing plan. The omission of a financing plan has drawn controversy, with critics charging that the Shumlin administration wants to avoid talking about what may be the largest tax increase in Vermont history. What the naysayers fail to mention, however, is that taxes would replace private insurance premiums and, by most estimates, Green Mountain Care would cover everyone for less total dollars than are currently spent in a system that leaves many uninsured.
The financing question has not been totally ignored. To fulfill a requirement of the new law, the Shumlin administration asked analysts at the University of Massachusetts to formulate baseline data for financing Green Mountain Care and to examine the financial implications of a federal health care exchange. The UMass report once again confirmed that a state single payer could cover everyone and still save money over the spending projections absent reform, but it stopped short of naming specific revenue sources, which was what single payer opponents had been clamoring for so that they could raise a hue and cry about taxes. Shumlin countered by pointing out that Green Mountain Care could not begin offering health coverage until 2017 at the earliest because of the Obamacare preemption, and therefore, he argued, a financing proposal would be premature.
Critics have also cried that doctors will leave the state when Green Mountain Care is implemented. Yet, while one or two specialists have indicated they might seek greener pastures elsewhere, there have been at least as many doctors outside the state who have said they would consider moving to Vermont so they could practice under a single payer system, and not have to worry about multiple insurance companies and whether their patients could afford needed care.
Vermont's efforts contain lessons for other states looking at enacting universal health care. The first lesson is that the design of a state-level system can be more complex than the design might be for a federal Medicare-for-all plan. For one thing, a state-level single payer must wrap around existing federal programs such as Medicare and Medicaid, or obtain waivers to capture the federal funds and apply them to the state plan. In addition, there are many cross-border issues that uniquely burden state-level initiatives. For instance, residents of one state may obtain health care services in another state. Others may live in one state but work in another. The question then becomes how to negotiate and pay for out-of-state services and how to adjust tax exposure for residents who may have out-of-state insurance. Finally, there is the question of the Employee Retirement Income Security Act (ERISA), the federal law that allows large employers to self-insure. ERISA prohibits states from interfering in self-insure health plans, but would probably not preclude a state payroll tax on all employers to support a universal health care plan. This would leave ERISA employers with the decision of whether to drop their self-insurance or try to challenge the payroll tax in federal court. No one, not even Hsiao, has been able to predict the outcome of a legal challenge to single payer financing based on the ERISA law. It remains one of the unknowns for Vermont going forward.
Vermont's single payer supporters have caught their breath, but have not exactly relaxed their efforts in advocating for the ultimate goal. The implementation of Obamacare in 2014 will be closely watched, as will the state's roll-out of the single payer benefits package and financing plan. Well-funded attacks on the Vermont single payer initiative have already been launched by political action committees and by Governor Shumlin's political opponents. These attacks play on the public's fear of change. But Vermonters are independent thinkers, and the single payer advocates have been quickly responding to the naysayers with letters to the editor and press releases reiterating the well-researched projections showing that single payer will save money.
The grand vision of Green Mountain Care continues to hold great promise: To treat all human beings as equals when it comes to necessary health care; to end the absurd spiral of health care costs that is crippling businesses, bankrupting school and municipal budgets, and threatening the entire economy; and to give doctors the ability to practice the kind of medicine for which they were trained--focusing on patients' needs, not on billing, insurance, and a patients' financial status. A majority of Vermonters are cautiously optimistic that, in four years, their state will become the first place in America to realize this dream.
In 1998, Dr. Deb Richter began, almost single handedly, to revive the dream of universal health care in the United States--open to all and paid for by the government. A primary care physician from Buffalo, New York, Richter had become outraged by the barriers to accessing quality health care in the city's low-income communities.
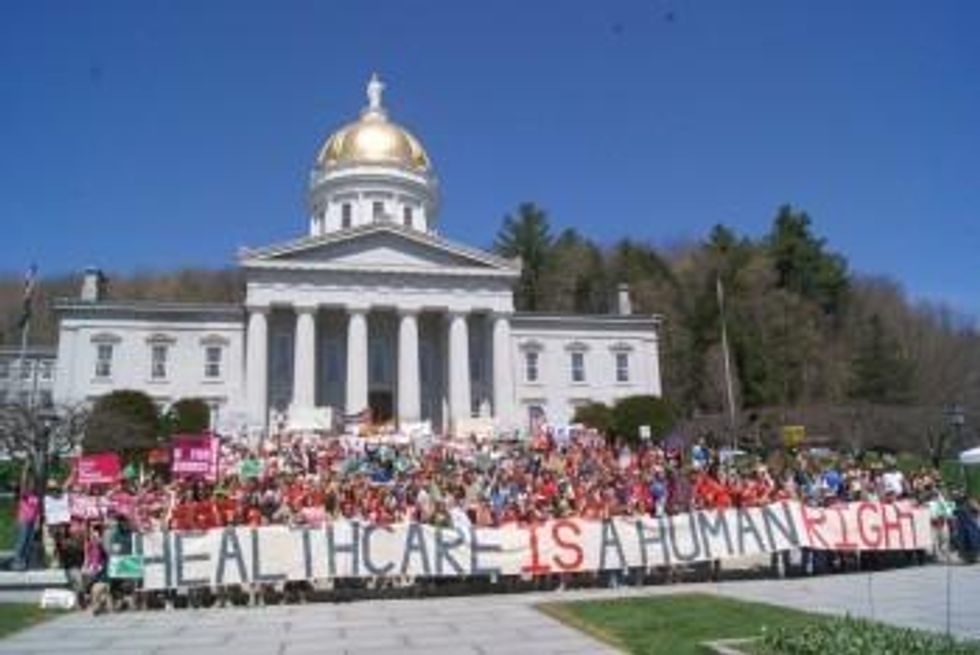
The existing system of privatized health care was expensive, opaque, and unfair, and yet reforming health care--as President Obama has discovered--means taking on a multi-billion dollar insurance industry that vociferously lobbies to maintain its profits.
Despairing of ever advancing universal care in the state of New York, Dr. Richter moved to Vermont where she thought that politics were on a scale where she could have an impact. Practicing medicine three days a week, Dr. Richter used the rest of her time to travel the state speaking about a so-called single payer system that would dispose of the multitude of private insurance companies and offer patients a simple point-of-access health care. Recognizing that businesses and doctors were key constituencies, she spoke to every Rotary Club and every business association that would have her, as well as to any doctor who would listen. She also started a new organization devoted solely to educating the public about the single payer system. She helped organize a rally that drew 1,000 people to the state capital. Eventually, Dr. Richter found her way inside the statehouse, where she formed alliances with legislators from all three parties--Democrat, Republican, and Progressive.
In 2011, with Dr. Richter standing by the Governor's side as he signed the bill, Vermont became the first state to enact a framework and a timetable for a state-level single payer health system. Implementation of the law now waits for the clearance of a number of crucial hurdles, among them a federal waiver of requirements in the Patient Protection and Affordable Care Act--Obamacare--and the passage of a financing plan that would raise enough new tax revenue to replace what is currently spent on private health insurance premiums.
Obamacare has been criticized by both the left and right for its failure to simplify the system or curb costs. There is a certain irony in the fact that President Obama's reforms-- which left the private insurance industry untouched and failed to introduce a "public option" that would force private insurers to lower their prices--might derail the Vermont initiative, which is designed to do both. Vermont's single payer plan would eliminate the private health care exchanges in which the uninsured will be mandated to buy insurance or pay a fine under Obamacare. Instead, Vermont would provide publicly funded health care for all residents. Federal law dictates that in order to do this, Vermont must obtain a waiver from the U.S. Secretary of Health and Human Services sanctioning the state initiative, thus enabling Vermont to continue receiving the federal dollars that would have subsidized the exchange. That remains a hurdle, but the state legislators shaping the bill are confident they will get the waiver.
Financing the single payer system is the other challenge. Vermont's lawmakers have until 2017--when the reforms come in effect--to raise $1.6 billion in new taxes to replace private insurance premiums and to cover the health care costs of those who are now uninsured. That presents a formidable challenge for a cash-strapped rural economy. Vermont already has some of the highest taxes in the country, although it has weathered the financial crisis more successfully than its southern neighbors by avoiding a housing bubble. New taxes might mean a 1 percent assessment on individuals' gross incomes and a 6--8.5 percent payroll tax. Local polling suggests that Vermonters are happy to pay more, provided additional revenue is ringfenced for health care.
The challenges are steep, but Vermont stands on the verge of a historic change--one that would make it the first U.S. state to have a universal health care system that is comparable with other developed countries. Could this be a tipping point in the battle against America epic health care problems? Could it also be the story of how an impassioned few succeeded in transforming their community?

Chris Wood, one of the original activists, said he was drawn to the concept of single payer because it was based on the premise that health care is a public good, comparable to public schools and fire departments. "It didn't make much sense to me," said Wood, "that something as important as health care should be left to the marketplace, where your wealth or your income might determine the kind of care you [are] able to get."
Wood and the other activists realized that neither the "crisis" nor its perceived solution were new. Norway has had a single payer health care system since 1912; Japan has had one since 1938. The United Kingdom began its single payer in 1948; Canada implemented one in 1966; and Taiwan did so in 1995. While all these countries pay for health care from a single government fund, the delivery system varies from country to country. In the U.K., the government not only finances health care, it also provides it through a national health service. On the other hand, Canada's single payer financing is funneled to private sector hospitals and physicians.
The total number of single payer countries around the world is hard to estimate because the term is not uniformly defined. Using the purest definition, only about 20 countries are truly single payer, the vast majority in the developed world. However, there are scores of countries, such as France and the Netherlands, which use a single payer to finance a basic benefit package for all citizens while allowing private or employment-based financing to cover additional services. Other countries, such as Switzerland and Germany, are generally thought to have multi-payer systems because they rely heavily on employment-based "sickness funds." However, the sickness funds are almost instrumentalities of the government because they are so tightly regulated and therefore bear little resemblance to for-profit U.S. insurance companies. Thus, among developed countries, only the U.S. fails to use the power of government to ensure health care access for all of its people. At the same time, the U.S. is the biggest spender on health care.
Although the U.S. made an important step toward universal care in 1965 with the enactment of Medicare and Medicaid, Obamacare is the only significant reform to have happened since, and many expect that Obamacare will fall short of providing universal access and controlling costs. Medicare, on the other hand, has been relatively successful in holding down costs. It pays providers according to a fixed fee schedule, and incurs administrative expenses of only 3.1 percent, compared to an average of 14.1 percent for private insurance, according to a 2005 study by the American Medical Association. But Medicare leaves out everyone under age 65 and Medicaid only covers the very poor. By the 1970s, many people who were not eligible for either federal program were finding that health care expenses, even with insurance, put them at serious financial risk.
In 1972, Senator Edward Kennedy authored the book In Critical Condition: The Crisis in America's Health Care. The book was based on the testimony of people Kennedy had invited to speak at Senate subcommittee hearings. Witnesses told of becoming pauperized from medical debt. They spoke of the unaffordability of health insurance, and decried the indignity of charity care. They chronicled the difficulty of finding doctors in low-income neighborhoods, and of navigating the confusing maze of services and insurance coverage. Others testified that they had trouble receiving good care, that the health care industry was profit-oriented and monopolistic, and that they had no say in the quality or availability of health care services.
Kennedy contrasted U.S. health care with what he had seen in trips to Sweden, Denmark, Norway, and Israel, and with what he had learned about the United Kingdom. "Most of us have been led to believe that health care is a disaster in Europe," he wrote. "From what I saw, these things are simply false. The fact is, while most Americans are angry and frustrated about health care, most Englishmen, Danes, Swedes, and Israelis are not." Kennedy concluded his book by calling for a program in which "the federal government would become the health insurance carrier for the entire nation." Kennedy was proposing a single payer system, although he did not use that term.

In 1988, 10 percent of Vermonters had no health insurance; thousands more were underinsured. Farmers, loggers, artists, or convenience store owners who got seriously ill often faced financial ruin. The access crisis--a plight shared by other U.S. states--was compounded by health care costs that were rising at greater than the inflation rate. Employers and individuals often saw double digit annual increases in insurance premiums, and those without insurance who attempted to pay hospital bills out of pocket paid the highest rates of all. The health care system was also rife with excessive administrative costs related to its fragmented financing streams. Providers had to deal with scores of payers--insurance companies, multiple insurance policies, federal and state health plans, and private individuals. The insurance industry in particular added immense cost to the system without adding anything of value in terms of health care. Furthermore, the fragmentation of financing meant that payers had little bargaining power in purchasing pharmaceuticals or medical equipment, nor any say in hospital spending. As costs kept escalating, any attempt to curtail spending in one area simply caused an increase in charges somewhere else.
However, because the U.S. Congress showed no inclination to consider reforms resembling the universal health care systems in other developed countries, the health care activists in Vermont concluded that state-level initiatives were the only hope. The activists told themselves that the momentum for reform builds over time, but when the time is ripe, change happens with surprising speed. The important thing was to have thought through the solution and to have educated the public about its merits, so that when the opportune moment arrived, a reorganized health care system would reveal itself as the most practical response.
In 1989, they established a small nonprofit called the Vermont Consumers' Campaign for Health. They raised funds, hired staff, and built a citizens' movement. They sponsored educational forums around the state, published a newsletter, and arranged meetings with labor unions, consumer groups, businesses, teachers, town officials, and politicians. The organization coordinated referenda on single payer health care at more than 50 town meetings, and drummed up support for a single payer bill to be introduced in the Vermont legislature.
The response to the group's efforts was overwhelmingly positive. Vermonters readily accepted the notion that the state should be everyone's health insurer. Businesses would be relieved of the burden of buying health insurance for employees. Labor unions would no longer have to fight for health benefits at every contract negotiation. All Vermonters would share in financing the program, and therefore all Vermonters would have a stake in ensuring its quality and efficiency.
However, the populace was ahead of its elected officials on the issue. Although single payer advocates had a big ally in Vermont's Independent former-Congressman Bernie Sanders, who had been busy in Washington trying to advance a national single payer proposal, Sanders' enthusiasm was not shared by state legislators. The health care committee chairpersons felt that other matters were more pressing and less politically charged. Thus, the first single payer bill to be introduced in the legislature (in 1991) never even got a committee hearing. The following year, former-Governor Howard Dean, himself a physician, failed to back the proposals, perhaps with an eye to his later presidential bid that was well-funded by the insurance industry.
The mid-90s saw increased focus on health care at the national level. The Clinton administration was promoting health reform based on "managed competition" among private insurers. Ultimately the effort was easily defeated by Congress. Meanwhile, in Vermont, a tiny minority of Progressive Party lawmakers finally succeeded in forcing a vote on the single payer system, but fell short. Instead, the idea of "managed care" was adopted in Vermont and elsewhere, a system that saved money for a year or two before simply becoming a vehicle for denying care and increasing insurance company profits. Consumers reacted by demanding a return to more traditional insurance policies.
The single payer movement might have died then and there, if not for the campaigning of Dr. Richter at the turn of the millennium. The need to corral costs had never been so urgent. Vermont's overall health care expenditures had doubled in less than 10 years. Health care had become a $5 billion per year industry in Vermont--19 percent of the gross domestic product. Yet, Vermont's governor at the time--Republican Jim Douglas--continued to oppose reform, even though a new state-commissioned study in 2001 showed that single payer would save $118 million annually, roughly a 5 percent reduction in Vermont's total health care spending.
It wasn't until 2010 that State Senator Peter Shumlin, also a gubernatorial candidate, dared to make the single payer system a centerpiece of his primary campaign. Shumlin had voted for the earlier single payer proposal, and had helped the legislature appropriate money for a Harvard professor, William Hsiao, to design an exhaustive study of how a universal health care system in Vermont might work.
Shumlin faced an uphill battle as polls showed him trailing his competitors early in the primary season. That's when Dr. Richter and a Middlebury College professor, Ellen Oxfeld, kicked into action--day after day on the phone, sending emails, attending meetings, pleading with friends and colleagues to support the single payer candidate. If Shumlin won, they said, Vermont would have a chance to lead the nation toward universal health care, just as Saskatchewan had led Canada to single payer decades before. People listened--and voted. Shumlin narrowly won the nomination, then went on to defeat his Republican opponent in the general election.
"The grassroots support I got from single payer advocates made it possible for me to be governor," Shumlin told an interviewer from Vermont Life magazine. "They knocked on doors. They poured their hearts out. They saw an opportunity and I would not be here without them."
As Shumlin took office, Professor Hsiao issued his report containing designs of three models that built on the state's previous reform efforts: a government-run single payer, a public option, and a public-private single payer that preserved some role for insurance companies in administering claims. It was this third option that was chosen, based on its eye-catch savings of 25 percent over the next decade. Hsiao attributed these savings to administrative simplification, reductions in fraud and abuse, reformed payment systems for doctors and hospitals, and no-fault medical malpractice reform.
Passage of a single payer bill was far from a sure thing, despite a democrat-controlled legislature. The major private health insurer in the state, Blue Cross Blue Shield, annually spends more on lobbying the state legislature than almost any other private firm. The pharmaceutical industry and the hospital association are not far behind. But with a population of only 600,000, Vermont's legislative process is so intimate that the voices of private citizens can sometimes have impact equal to the professional lobbyists. A cascade of concerned citizens flooded the statehouse in favor of single payer. Most visible were members of a "Health Care is a Human Right" campaign organized by the pro-labor Vermont Workers' Center. Wearing red t-shirts, they filled the committee rooms and visitors' galleries, watching every debate, and reading every mark-up of the bill. Dr. Richter's group was also present and single payer supporters throughout the state were kept up-to-date by email.
The bill that passed and was signed into law in the spring of 2011 laid the foundation for Green Mountain Care, the purpose of which was "to provide, as a public good, comprehensive, affordable, high quality, publicly financed health care coverage for all Vermont residents in a seamless and equitable manner regardless of income, assets, health status, or availability of other coverage." The law established a five-member board to oversee the program and administer payments to providers from a dedicated fund. The program would contain costs by reducing unnecessary administrative expenses and establishing innovative payment mechanisms to providers, such as global budgets to hospitals.
However, the law left several items of business unfinished. First was the uncertain interface with Obamacare, the federal health care law passed by Congress the previous fall. National health care reform was clearly headed in a different direction from Vermont's single payer system. Obamacare will require all individuals to have insurance by 2014. Those not covered by Medicare or Medicaid must purchase private insurance in health care "exchanges." Federal subsidies will be available to individuals who qualify on the basis of income. No state may proceed in a different manner unless granted a federal waiver, and Obamacare explicitly prohibits waivers until 2017 at the earliest. That means that implementation of Green Mountain Care will have to wait.
Second, the Vermont law did not include a benefits package or a financing plan. The omission of a financing plan has drawn controversy, with critics charging that the Shumlin administration wants to avoid talking about what may be the largest tax increase in Vermont history. What the naysayers fail to mention, however, is that taxes would replace private insurance premiums and, by most estimates, Green Mountain Care would cover everyone for less total dollars than are currently spent in a system that leaves many uninsured.
The financing question has not been totally ignored. To fulfill a requirement of the new law, the Shumlin administration asked analysts at the University of Massachusetts to formulate baseline data for financing Green Mountain Care and to examine the financial implications of a federal health care exchange. The UMass report once again confirmed that a state single payer could cover everyone and still save money over the spending projections absent reform, but it stopped short of naming specific revenue sources, which was what single payer opponents had been clamoring for so that they could raise a hue and cry about taxes. Shumlin countered by pointing out that Green Mountain Care could not begin offering health coverage until 2017 at the earliest because of the Obamacare preemption, and therefore, he argued, a financing proposal would be premature.
Critics have also cried that doctors will leave the state when Green Mountain Care is implemented. Yet, while one or two specialists have indicated they might seek greener pastures elsewhere, there have been at least as many doctors outside the state who have said they would consider moving to Vermont so they could practice under a single payer system, and not have to worry about multiple insurance companies and whether their patients could afford needed care.
Vermont's efforts contain lessons for other states looking at enacting universal health care. The first lesson is that the design of a state-level system can be more complex than the design might be for a federal Medicare-for-all plan. For one thing, a state-level single payer must wrap around existing federal programs such as Medicare and Medicaid, or obtain waivers to capture the federal funds and apply them to the state plan. In addition, there are many cross-border issues that uniquely burden state-level initiatives. For instance, residents of one state may obtain health care services in another state. Others may live in one state but work in another. The question then becomes how to negotiate and pay for out-of-state services and how to adjust tax exposure for residents who may have out-of-state insurance. Finally, there is the question of the Employee Retirement Income Security Act (ERISA), the federal law that allows large employers to self-insure. ERISA prohibits states from interfering in self-insure health plans, but would probably not preclude a state payroll tax on all employers to support a universal health care plan. This would leave ERISA employers with the decision of whether to drop their self-insurance or try to challenge the payroll tax in federal court. No one, not even Hsiao, has been able to predict the outcome of a legal challenge to single payer financing based on the ERISA law. It remains one of the unknowns for Vermont going forward.
Vermont's single payer supporters have caught their breath, but have not exactly relaxed their efforts in advocating for the ultimate goal. The implementation of Obamacare in 2014 will be closely watched, as will the state's roll-out of the single payer benefits package and financing plan. Well-funded attacks on the Vermont single payer initiative have already been launched by political action committees and by Governor Shumlin's political opponents. These attacks play on the public's fear of change. But Vermonters are independent thinkers, and the single payer advocates have been quickly responding to the naysayers with letters to the editor and press releases reiterating the well-researched projections showing that single payer will save money.
The grand vision of Green Mountain Care continues to hold great promise: To treat all human beings as equals when it comes to necessary health care; to end the absurd spiral of health care costs that is crippling businesses, bankrupting school and municipal budgets, and threatening the entire economy; and to give doctors the ability to practice the kind of medicine for which they were trained--focusing on patients' needs, not on billing, insurance, and a patients' financial status. A majority of Vermonters are cautiously optimistic that, in four years, their state will become the first place in America to realize this dream.