

SUBSCRIBE TO OUR FREE NEWSLETTER
Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
5
#000000
#FFFFFF
To donate by check, phone, or other method, see our More Ways to Give page.


Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
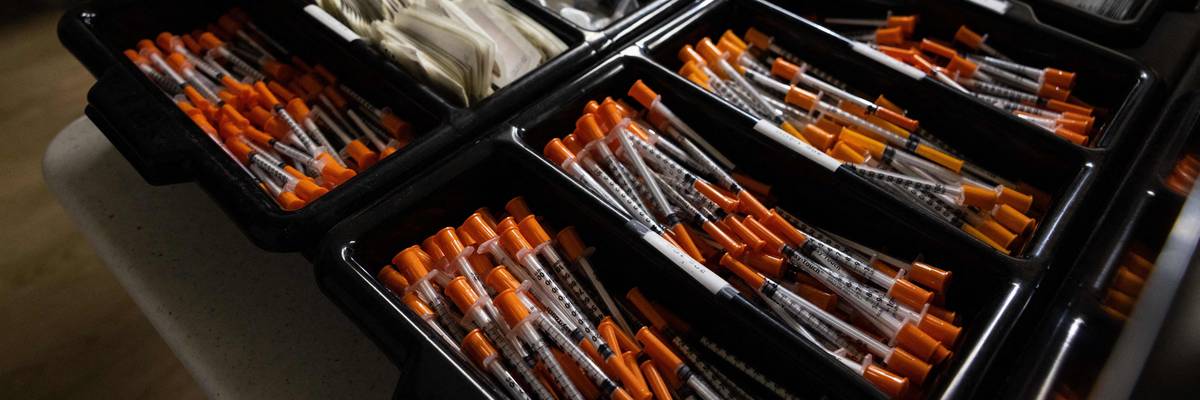
In this November 30, 2021 photo, syringes and other medical equipment are shown during the media tour of their supervised drug injection site OnPoint, in New York. Operated by OnPoint NYC, a consortium of two nonprofit social welfare organizations, these centers are the first to be officially licensed in the United States. They offer opioid and other drug users a variety of services, including addiction treatment.
We have come too far to turn our backs on what works when it comes to sound, life-saving drug policies. Now is the wrong time to politicize practical, proven responses to this medical emergency.
We lost more than 80,000 Americans to overdose last year, making it the leading cause of death for adults aged 18 to 44. But, for the first time in years, we have some reason for hope: in 2024, overdose deaths dropped by 27 percent. That progress, however, didn’t happen on its own. It came from investments in harm reduction: an ecosystem of strategies including naloxone distribution, syringe service programs, medications for opioid use disorder, and housing-first programs that secured shelter for people before connecting them to care.
Unfortunately, much of that progress is in danger. In recent weeks, President Trump issued an executive order targeting the very programs that provide these services and helped bring down overdose deaths. In doing so, the administration is cutting federal funding for proven, evidence-based interventions. It is also carving out naloxone from the larger harm reduction ecosystem it belongs to, falsely suggesting that naloxone can succeed in isolation. The reality is that saving someone from an overdose requires more than just increasing naloxone’s availability. It requires a broader public health approach to reach those at risk. Without systemic support for trusted community-led networks, naloxone will not be able to reach the people who are most vulnerable.
I should know. I’ve spent the past 30 years working with people who use drugs—first addressing HIV in Central and Eastern Europe, and now as Director of Drug Policy at the Open Society Foundations, where we support harm reduction efforts globally. I’ve seen, time and again, that when we lead with evidence and compassion, we save lives.
The biggest barrier we consistently face isn’t science, but the stigma and misunderstandings associated with drug use.
Back in the 1990s, I worked on a program that supported harm reduction efforts in former Soviet countries, then the region with the highest rates of HIV among people who use drugs. The interventions were straightforward: provide sterile syringes, educate people about safe injections, and offer access to basic medical care. Whether in Tomsk, Russia, or my hometown in New Jersey, I never met a person who didn’t want to protect themselves. We were fortunate to have tools that people actually wanted. And they work. Syringe service programs cut HIV and hepatitis C infections in half. Other interventions, like methadone and buprenorphine, can lower HIV incidence by as much as 60 percent by helping people reduce or stop injecting altogether.
The biggest barrier we consistently face isn’t science, but the stigma and misunderstandings associated with drug use.
People mistakenly believe that providing sterile syringes encourages drug use or that drug treatment medications simply “replace one drug with another.” But by supporting and translating scientific research, educating medical professionals, and, perhaps most importantly, supporting people who use drugs, we’ve made great progress. These efforts have not only produced strong results but have also helped chip away at longstanding stigma.
Take, for example, the OnPoint NYC—the first overdose prevention center in the country. Since 2021, the center has reversed nearly 2,000 overdoses. Syringe exchange programs are now authorized in 37 states, the District of Columbia, and Puerto Rico. With bipartisan support, red states from Kentucky to Indiana to South Carolina are using opioid settlement funds to support critical harm reduction work. The reality that many have recognized is that harm reduction programs provide an important on-ramp to broader care. They engage people who often don’t go to traditional medical providers out of fear. People who visit syringe service programs are five times more likely to enter treatment than those who don’t. Harm reduction programs are an optimal venue for naloxone distribution since they directly reach people at risk of overdose. That’s why the Trump administration’s recent actions are so concerning. They reflect a shift away from science that has been working.
We have come too far to turn our backs on what works. We must not politicize practical, proven responses to this medical emergency. We live in a time where evidence-based public health interventions that had once been taken as givens have become political flashpoints. But we can’t let politics come in the way of saving very real lives. Too much is at stake now.
Dear Common Dreams reader, It’s been nearly 30 years since I co-founded Common Dreams with my late wife, Lina Newhouser. We had the radical notion that journalism should serve the public good, not corporate profits. It was clear to us from the outset what it would take to build such a project. No paid advertisements. No corporate sponsors. No millionaire publisher telling us what to think or do. Many people said we wouldn't last a year, but we proved those doubters wrong. Together with a tremendous team of journalists and dedicated staff, we built an independent media outlet free from the constraints of profits and corporate control. Our mission has always been simple: To inform. To inspire. To ignite change for the common good. Building Common Dreams was not easy. Our survival was never guaranteed. When you take on the most powerful forces—Wall Street greed, fossil fuel industry destruction, Big Tech lobbyists, and uber-rich oligarchs who have spent billions upon billions rigging the economy and democracy in their favor—the only bulwark you have is supporters who believe in your work. But here’s the urgent message from me today. It's never been this bad out there. And it's never been this hard to keep us going. At the very moment Common Dreams is most needed, the threats we face are intensifying. We need your support now more than ever. We don't accept corporate advertising and never will. We don't have a paywall because we don't think people should be blocked from critical news based on their ability to pay. Everything we do is funded by the donations of readers like you. When everyone does the little they can afford, we are strong. But if that support retreats or dries up, so do we. Will you donate now to make sure Common Dreams not only survives but thrives? —Craig Brown, Co-founder |
We lost more than 80,000 Americans to overdose last year, making it the leading cause of death for adults aged 18 to 44. But, for the first time in years, we have some reason for hope: in 2024, overdose deaths dropped by 27 percent. That progress, however, didn’t happen on its own. It came from investments in harm reduction: an ecosystem of strategies including naloxone distribution, syringe service programs, medications for opioid use disorder, and housing-first programs that secured shelter for people before connecting them to care.
Unfortunately, much of that progress is in danger. In recent weeks, President Trump issued an executive order targeting the very programs that provide these services and helped bring down overdose deaths. In doing so, the administration is cutting federal funding for proven, evidence-based interventions. It is also carving out naloxone from the larger harm reduction ecosystem it belongs to, falsely suggesting that naloxone can succeed in isolation. The reality is that saving someone from an overdose requires more than just increasing naloxone’s availability. It requires a broader public health approach to reach those at risk. Without systemic support for trusted community-led networks, naloxone will not be able to reach the people who are most vulnerable.
I should know. I’ve spent the past 30 years working with people who use drugs—first addressing HIV in Central and Eastern Europe, and now as Director of Drug Policy at the Open Society Foundations, where we support harm reduction efforts globally. I’ve seen, time and again, that when we lead with evidence and compassion, we save lives.
The biggest barrier we consistently face isn’t science, but the stigma and misunderstandings associated with drug use.
Back in the 1990s, I worked on a program that supported harm reduction efforts in former Soviet countries, then the region with the highest rates of HIV among people who use drugs. The interventions were straightforward: provide sterile syringes, educate people about safe injections, and offer access to basic medical care. Whether in Tomsk, Russia, or my hometown in New Jersey, I never met a person who didn’t want to protect themselves. We were fortunate to have tools that people actually wanted. And they work. Syringe service programs cut HIV and hepatitis C infections in half. Other interventions, like methadone and buprenorphine, can lower HIV incidence by as much as 60 percent by helping people reduce or stop injecting altogether.
The biggest barrier we consistently face isn’t science, but the stigma and misunderstandings associated with drug use.
People mistakenly believe that providing sterile syringes encourages drug use or that drug treatment medications simply “replace one drug with another.” But by supporting and translating scientific research, educating medical professionals, and, perhaps most importantly, supporting people who use drugs, we’ve made great progress. These efforts have not only produced strong results but have also helped chip away at longstanding stigma.
Take, for example, the OnPoint NYC—the first overdose prevention center in the country. Since 2021, the center has reversed nearly 2,000 overdoses. Syringe exchange programs are now authorized in 37 states, the District of Columbia, and Puerto Rico. With bipartisan support, red states from Kentucky to Indiana to South Carolina are using opioid settlement funds to support critical harm reduction work. The reality that many have recognized is that harm reduction programs provide an important on-ramp to broader care. They engage people who often don’t go to traditional medical providers out of fear. People who visit syringe service programs are five times more likely to enter treatment than those who don’t. Harm reduction programs are an optimal venue for naloxone distribution since they directly reach people at risk of overdose. That’s why the Trump administration’s recent actions are so concerning. They reflect a shift away from science that has been working.
We have come too far to turn our backs on what works. We must not politicize practical, proven responses to this medical emergency. We live in a time where evidence-based public health interventions that had once been taken as givens have become political flashpoints. But we can’t let politics come in the way of saving very real lives. Too much is at stake now.
We lost more than 80,000 Americans to overdose last year, making it the leading cause of death for adults aged 18 to 44. But, for the first time in years, we have some reason for hope: in 2024, overdose deaths dropped by 27 percent. That progress, however, didn’t happen on its own. It came from investments in harm reduction: an ecosystem of strategies including naloxone distribution, syringe service programs, medications for opioid use disorder, and housing-first programs that secured shelter for people before connecting them to care.
Unfortunately, much of that progress is in danger. In recent weeks, President Trump issued an executive order targeting the very programs that provide these services and helped bring down overdose deaths. In doing so, the administration is cutting federal funding for proven, evidence-based interventions. It is also carving out naloxone from the larger harm reduction ecosystem it belongs to, falsely suggesting that naloxone can succeed in isolation. The reality is that saving someone from an overdose requires more than just increasing naloxone’s availability. It requires a broader public health approach to reach those at risk. Without systemic support for trusted community-led networks, naloxone will not be able to reach the people who are most vulnerable.
I should know. I’ve spent the past 30 years working with people who use drugs—first addressing HIV in Central and Eastern Europe, and now as Director of Drug Policy at the Open Society Foundations, where we support harm reduction efforts globally. I’ve seen, time and again, that when we lead with evidence and compassion, we save lives.
The biggest barrier we consistently face isn’t science, but the stigma and misunderstandings associated with drug use.
Back in the 1990s, I worked on a program that supported harm reduction efforts in former Soviet countries, then the region with the highest rates of HIV among people who use drugs. The interventions were straightforward: provide sterile syringes, educate people about safe injections, and offer access to basic medical care. Whether in Tomsk, Russia, or my hometown in New Jersey, I never met a person who didn’t want to protect themselves. We were fortunate to have tools that people actually wanted. And they work. Syringe service programs cut HIV and hepatitis C infections in half. Other interventions, like methadone and buprenorphine, can lower HIV incidence by as much as 60 percent by helping people reduce or stop injecting altogether.
The biggest barrier we consistently face isn’t science, but the stigma and misunderstandings associated with drug use.
People mistakenly believe that providing sterile syringes encourages drug use or that drug treatment medications simply “replace one drug with another.” But by supporting and translating scientific research, educating medical professionals, and, perhaps most importantly, supporting people who use drugs, we’ve made great progress. These efforts have not only produced strong results but have also helped chip away at longstanding stigma.
Take, for example, the OnPoint NYC—the first overdose prevention center in the country. Since 2021, the center has reversed nearly 2,000 overdoses. Syringe exchange programs are now authorized in 37 states, the District of Columbia, and Puerto Rico. With bipartisan support, red states from Kentucky to Indiana to South Carolina are using opioid settlement funds to support critical harm reduction work. The reality that many have recognized is that harm reduction programs provide an important on-ramp to broader care. They engage people who often don’t go to traditional medical providers out of fear. People who visit syringe service programs are five times more likely to enter treatment than those who don’t. Harm reduction programs are an optimal venue for naloxone distribution since they directly reach people at risk of overdose. That’s why the Trump administration’s recent actions are so concerning. They reflect a shift away from science that has been working.
We have come too far to turn our backs on what works. We must not politicize practical, proven responses to this medical emergency. We live in a time where evidence-based public health interventions that had once been taken as givens have become political flashpoints. But we can’t let politics come in the way of saving very real lives. Too much is at stake now.