

SUBSCRIBE TO OUR FREE NEWSLETTER
Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
5
#000000
#FFFFFF
To donate by check, phone, or other method, see our More Ways to Give page.


Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
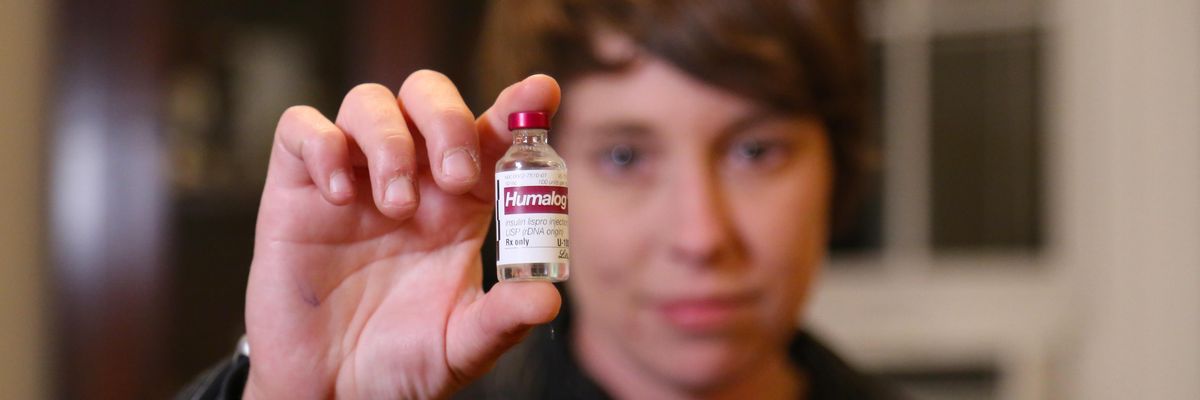
A patient holds a vial of Humalog, an insulin product made by Eli Lilly, on September 27, 2016.
"No one should be forced to ration or go without basic medication that could mean the difference between life or death," said California Attorney General Rob Bonta.
The California Justice Department on Thursday sued three large pharmaceutical companies as well as several major pharmacy benefit managers for unlawfully coordinating to drive up the cost of insulin, a lifesaving medication that patients in the United States are often forced to ration due to high prices.
"Insulin is a necessary drug that millions of Americans rely upon for their health, not a luxury good," California Attorney General Rob Bonta said in a statement announcing the lawsuit, which targets Eli Lilly, Novo Nordisk, and Sanofi—three of the largest insulin-makers in the world—and CVS Caremark, Express Scripts, and OptumRx.
The lawsuit accuses the companies of illegally leveraging their market dominance to push up prices, making insulin far more expensive in the U.S. than in Canada or other wealthy nations.
The California Justice Department points to a 2021 RAND Corporation study showing that the average price of all types of insulin in the U.S. is more than ten times higher than in Japan, Canada, Germany, France, and other countries.
"The average list price for a vial of insulin in Canada was $12," the study noted. "Step across the border into America, and it's $98.70."
A separate study published in the Annals of Internal Medicine in October estimated that roughly 1.3 million U.S. adults with diabetes either skipped insulin doses, took less than they needed, or delayed purchases of the medicine over the previous 12 months due to its high cost. Forgoing prescribed insulin doses can have fatal consequences.
"No one should be forced to ration or go without basic medication that could mean the difference between life or death," Bonta said Thursday. "California will continue to be a leader in the fight to ensure everyone has equal access to affordable healthcare and prescription medications they need to stay healthy."
"The United States insulin market is an oligopoly."
According to the California DOJ, Eli Lilly, Novo Nordisk, and Sanofi produce more than 90% of the global insulin supply. The pharmacy benefit managers (PBMs) CVS Caremark, Express Scripts, and OptumRx, meanwhile, "administer pharmacy benefits for roughly 80% of prescription claims managed."
"The United States insulin market is an oligopoly," the new lawsuit states. "The manufacturer defendants aggressively raise the list price of insulin in lockstep with each other to artificial levels. The inflated and artificial insulin price increases have significantly exceeded inflation and are not justified by advances in the efficacy of the drugs or the cost of manufacturing. Insulin costs less than $10 a month to manufacture and its development costs have long been recouped."
"PBM defendants obtain significant secret rebates, which are a percentage of the inflated and artificial list price, from the manufacturer defendants in exchange for favorable placement on the PBMs' standard formularies," the complaint continues. "This rebating strategy incentivizes the manufacturer defendants to raise their list prices high and higher. The result is that the PBM
defendants' standard formularies promote the Manufacturer Defendants’ high list-price insulin products over lower list-price insulins in California and nationwide."
The state's lawsuit—which resembles legal action recently taken by Arkansas, Kansas, and Mississippi—demands that the pharmaceutical giants and PBMs be "permanently enjoined from committing any acts of unfair competition" and requests a court order "awarding all equitable monetary relief available from defendants as a result of their acts of unjust enrichment."
Insulin prices in the U.S. have long been viewed as a scandal—one of the many negative consequences of allowing pharmaceutical companies to price gouge at will. California has announced plans to manufacture its own low-cost insulin as an alternative to the private market.
Last year, Human Rights Watch released a report that spotlighted the pricing practices of the trio of insulin makers at the center of California's new lawsuit.
The report found that "when adjusted for inflation, Eli Lilly’s list price for Humalog increased by about 680%, to $275 per vial in 2018, since it first began selling in the US in 1996."
"The inflation-adjusted list price for Novo Nordisk’s Novolog rose about 403% to about $289 per vial, between its market entry in 2000 and 2018," the rights group noted. "Similarly, Sanofi's list price for Lantus rose about 420% when adjusted for inflation since its US market entry in 2000, to about $276 per vial in 2019."
Though the recently passed Inflation Reduction Act includes a $35-per-month cap on insulin copayments, it only applies to Medicare recipients, leaving out the majority of people in the U.S. with diabetes.
Dear Common Dreams reader, It’s been nearly 30 years since I co-founded Common Dreams with my late wife, Lina Newhouser. We had the radical notion that journalism should serve the public good, not corporate profits. It was clear to us from the outset what it would take to build such a project. No paid advertisements. No corporate sponsors. No millionaire publisher telling us what to think or do. Many people said we wouldn't last a year, but we proved those doubters wrong. Together with a tremendous team of journalists and dedicated staff, we built an independent media outlet free from the constraints of profits and corporate control. Our mission has always been simple: To inform. To inspire. To ignite change for the common good. Building Common Dreams was not easy. Our survival was never guaranteed. When you take on the most powerful forces—Wall Street greed, fossil fuel industry destruction, Big Tech lobbyists, and uber-rich oligarchs who have spent billions upon billions rigging the economy and democracy in their favor—the only bulwark you have is supporters who believe in your work. But here’s the urgent message from me today. It's never been this bad out there. And it's never been this hard to keep us going. At the very moment Common Dreams is most needed, the threats we face are intensifying. We need your support now more than ever. We don't accept corporate advertising and never will. We don't have a paywall because we don't think people should be blocked from critical news based on their ability to pay. Everything we do is funded by the donations of readers like you. When everyone does the little they can afford, we are strong. But if that support retreats or dries up, so do we. Will you donate now to make sure Common Dreams not only survives but thrives? —Craig Brown, Co-founder |
The California Justice Department on Thursday sued three large pharmaceutical companies as well as several major pharmacy benefit managers for unlawfully coordinating to drive up the cost of insulin, a lifesaving medication that patients in the United States are often forced to ration due to high prices.
"Insulin is a necessary drug that millions of Americans rely upon for their health, not a luxury good," California Attorney General Rob Bonta said in a statement announcing the lawsuit, which targets Eli Lilly, Novo Nordisk, and Sanofi—three of the largest insulin-makers in the world—and CVS Caremark, Express Scripts, and OptumRx.
The lawsuit accuses the companies of illegally leveraging their market dominance to push up prices, making insulin far more expensive in the U.S. than in Canada or other wealthy nations.
The California Justice Department points to a 2021 RAND Corporation study showing that the average price of all types of insulin in the U.S. is more than ten times higher than in Japan, Canada, Germany, France, and other countries.
"The average list price for a vial of insulin in Canada was $12," the study noted. "Step across the border into America, and it's $98.70."
A separate study published in the Annals of Internal Medicine in October estimated that roughly 1.3 million U.S. adults with diabetes either skipped insulin doses, took less than they needed, or delayed purchases of the medicine over the previous 12 months due to its high cost. Forgoing prescribed insulin doses can have fatal consequences.
"No one should be forced to ration or go without basic medication that could mean the difference between life or death," Bonta said Thursday. "California will continue to be a leader in the fight to ensure everyone has equal access to affordable healthcare and prescription medications they need to stay healthy."
"The United States insulin market is an oligopoly."
According to the California DOJ, Eli Lilly, Novo Nordisk, and Sanofi produce more than 90% of the global insulin supply. The pharmacy benefit managers (PBMs) CVS Caremark, Express Scripts, and OptumRx, meanwhile, "administer pharmacy benefits for roughly 80% of prescription claims managed."
"The United States insulin market is an oligopoly," the new lawsuit states. "The manufacturer defendants aggressively raise the list price of insulin in lockstep with each other to artificial levels. The inflated and artificial insulin price increases have significantly exceeded inflation and are not justified by advances in the efficacy of the drugs or the cost of manufacturing. Insulin costs less than $10 a month to manufacture and its development costs have long been recouped."
"PBM defendants obtain significant secret rebates, which are a percentage of the inflated and artificial list price, from the manufacturer defendants in exchange for favorable placement on the PBMs' standard formularies," the complaint continues. "This rebating strategy incentivizes the manufacturer defendants to raise their list prices high and higher. The result is that the PBM
defendants' standard formularies promote the Manufacturer Defendants’ high list-price insulin products over lower list-price insulins in California and nationwide."
The state's lawsuit—which resembles legal action recently taken by Arkansas, Kansas, and Mississippi—demands that the pharmaceutical giants and PBMs be "permanently enjoined from committing any acts of unfair competition" and requests a court order "awarding all equitable monetary relief available from defendants as a result of their acts of unjust enrichment."
Insulin prices in the U.S. have long been viewed as a scandal—one of the many negative consequences of allowing pharmaceutical companies to price gouge at will. California has announced plans to manufacture its own low-cost insulin as an alternative to the private market.
Last year, Human Rights Watch released a report that spotlighted the pricing practices of the trio of insulin makers at the center of California's new lawsuit.
The report found that "when adjusted for inflation, Eli Lilly’s list price for Humalog increased by about 680%, to $275 per vial in 2018, since it first began selling in the US in 1996."
"The inflation-adjusted list price for Novo Nordisk’s Novolog rose about 403% to about $289 per vial, between its market entry in 2000 and 2018," the rights group noted. "Similarly, Sanofi's list price for Lantus rose about 420% when adjusted for inflation since its US market entry in 2000, to about $276 per vial in 2019."
Though the recently passed Inflation Reduction Act includes a $35-per-month cap on insulin copayments, it only applies to Medicare recipients, leaving out the majority of people in the U.S. with diabetes.
The California Justice Department on Thursday sued three large pharmaceutical companies as well as several major pharmacy benefit managers for unlawfully coordinating to drive up the cost of insulin, a lifesaving medication that patients in the United States are often forced to ration due to high prices.
"Insulin is a necessary drug that millions of Americans rely upon for their health, not a luxury good," California Attorney General Rob Bonta said in a statement announcing the lawsuit, which targets Eli Lilly, Novo Nordisk, and Sanofi—three of the largest insulin-makers in the world—and CVS Caremark, Express Scripts, and OptumRx.
The lawsuit accuses the companies of illegally leveraging their market dominance to push up prices, making insulin far more expensive in the U.S. than in Canada or other wealthy nations.
The California Justice Department points to a 2021 RAND Corporation study showing that the average price of all types of insulin in the U.S. is more than ten times higher than in Japan, Canada, Germany, France, and other countries.
"The average list price for a vial of insulin in Canada was $12," the study noted. "Step across the border into America, and it's $98.70."
A separate study published in the Annals of Internal Medicine in October estimated that roughly 1.3 million U.S. adults with diabetes either skipped insulin doses, took less than they needed, or delayed purchases of the medicine over the previous 12 months due to its high cost. Forgoing prescribed insulin doses can have fatal consequences.
"No one should be forced to ration or go without basic medication that could mean the difference between life or death," Bonta said Thursday. "California will continue to be a leader in the fight to ensure everyone has equal access to affordable healthcare and prescription medications they need to stay healthy."
"The United States insulin market is an oligopoly."
According to the California DOJ, Eli Lilly, Novo Nordisk, and Sanofi produce more than 90% of the global insulin supply. The pharmacy benefit managers (PBMs) CVS Caremark, Express Scripts, and OptumRx, meanwhile, "administer pharmacy benefits for roughly 80% of prescription claims managed."
"The United States insulin market is an oligopoly," the new lawsuit states. "The manufacturer defendants aggressively raise the list price of insulin in lockstep with each other to artificial levels. The inflated and artificial insulin price increases have significantly exceeded inflation and are not justified by advances in the efficacy of the drugs or the cost of manufacturing. Insulin costs less than $10 a month to manufacture and its development costs have long been recouped."
"PBM defendants obtain significant secret rebates, which are a percentage of the inflated and artificial list price, from the manufacturer defendants in exchange for favorable placement on the PBMs' standard formularies," the complaint continues. "This rebating strategy incentivizes the manufacturer defendants to raise their list prices high and higher. The result is that the PBM
defendants' standard formularies promote the Manufacturer Defendants’ high list-price insulin products over lower list-price insulins in California and nationwide."
The state's lawsuit—which resembles legal action recently taken by Arkansas, Kansas, and Mississippi—demands that the pharmaceutical giants and PBMs be "permanently enjoined from committing any acts of unfair competition" and requests a court order "awarding all equitable monetary relief available from defendants as a result of their acts of unjust enrichment."
Insulin prices in the U.S. have long been viewed as a scandal—one of the many negative consequences of allowing pharmaceutical companies to price gouge at will. California has announced plans to manufacture its own low-cost insulin as an alternative to the private market.
Last year, Human Rights Watch released a report that spotlighted the pricing practices of the trio of insulin makers at the center of California's new lawsuit.
The report found that "when adjusted for inflation, Eli Lilly’s list price for Humalog increased by about 680%, to $275 per vial in 2018, since it first began selling in the US in 1996."
"The inflation-adjusted list price for Novo Nordisk’s Novolog rose about 403% to about $289 per vial, between its market entry in 2000 and 2018," the rights group noted. "Similarly, Sanofi's list price for Lantus rose about 420% when adjusted for inflation since its US market entry in 2000, to about $276 per vial in 2019."
Though the recently passed Inflation Reduction Act includes a $35-per-month cap on insulin copayments, it only applies to Medicare recipients, leaving out the majority of people in the U.S. with diabetes.