

SUBSCRIBE TO OUR FREE NEWSLETTER
Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
5
#000000
#FFFFFF
To donate by check, phone, or other method, see our More Ways to Give page.


Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
Bolstering the call for universal coverage and undercutting a key Republican talking point, a new study finds that Medicaid expansion in Arkansas and Kentucky resulted in better healthcare and improved health outcomes among low-income Americans.
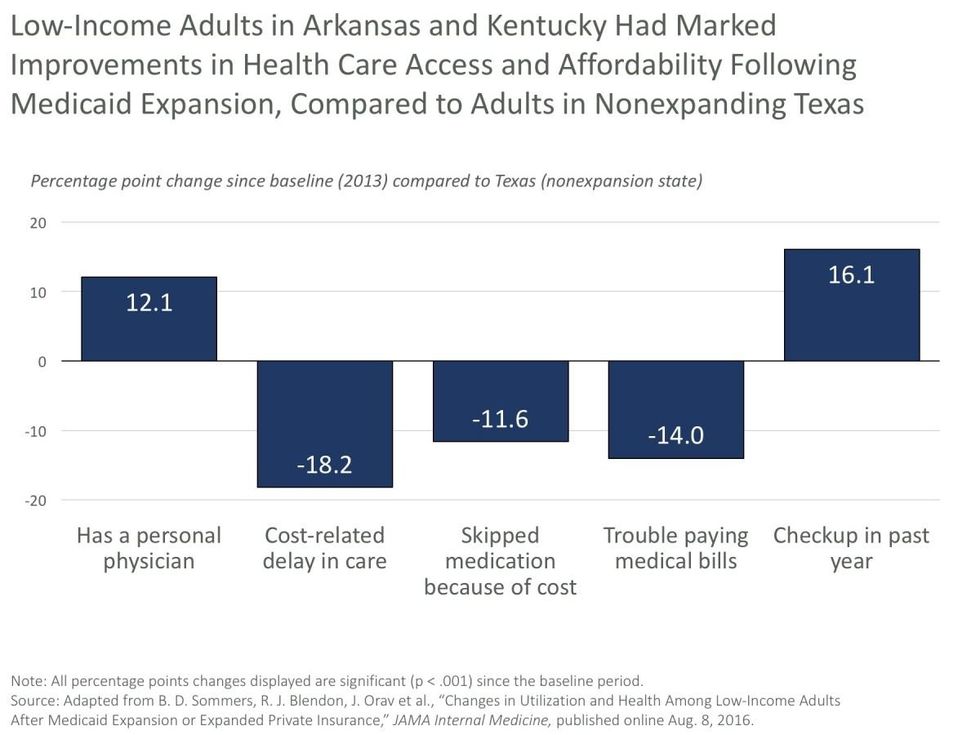
The research from the Harvard T.H. Chan School of Public Health shows that two years after Medicaid coverage was expanded under the Affordable Care Act (ACA) in their states, low-income adults in Kentucky and Arkansas received more primary and preventive care, made fewer emergency room visits, had less trouble paying bills, and reported higher quality care and improved health compared with their counterparts in Texas, one of 19 states that did not expand Medicaid.
"Medicaid is our nation's strongest tool to combat health disparities, moving us, albeit slowly, toward a day when all people have the ability to attain the highest level of health."
--Elizabeth Taylor, National Health Law Program
The findings came out Monday in the journal JAMA Internal Medicine.
According to a press statement, lead study author Benjamin Sommers and colleagues surveyed approximately 9,000 low-income adults in Arkansas, Kentucky, and Texas from late 2013 to the end of 2015:
The results showed that, between 2013 and 2015, the uninsured rate dropped from 42 percent to 14 percent in Arkansas and from 40 percent to 9 percent in Kentucky, compared with a much smaller change in Texas (39 percent to 32 percent). Expansion also was associated with significantly increased access to primary care, improved affordability of medications, reduced out-of-pocket spending, reduced likelihood of emergency department visits, and increased outpatient visits. Screening for diabetes, glucose testing among people with diabetes, and regular care for chronic conditions all increased significantly after expansion. Quality of care ratings improved significantly, as did the number of adults reporting excellent health.
The researchers found similar benefits for residents in Kentucky--which expanded traditional Medicaid--and Arkansas, which used federal Medicaid funding to subsidize private insurance, the so-called "private option."
This led Sommers, who teaches at both the Chan School and Harvard Medical School, to declare: "What this means is that it doesn't matter so much how states expand coverage. What matters is whether they expand at all."
Local station WFPL notes:
The results of the new study come as the [Kentucky Gov. Matt] Bevin administration is still sorting through comments on its proposed Medicaid expansion waiver. If approved as-is, it would put in place monthly premiums for individuals earning more than $11,880, co-pays for people earning less than the federal poverty limit, and eliminate default vision and dental coverage for able-bodied adults. Bevin is proposing a 'rewards' account that would let people earn points toward those benefits.
Of Bevin's waiver application, the Kentucky Center for Economic Policy said last month:
The proposed changes will result in fewer Kentuckians covered and decrease health care access, which will ultimately harm the health status of Kentuckians and move the state backwards in its recent health care gains. And while the proposal is framed in terms of increased financial sustainability and reduced costs, it can end up costing the state more overall as it introduces new, expensive and complex administrative burdens, and limits access to the preventative care that improves health. In the end, rolling back Kentucky's historic gains in healthcare coverage would be antithetical to the goals of the Medicaid program [...] and hurt the many Kentuckians who benefit from the Medicaid program in its current form.
"We need to get everyone covered in a single-payer system, but until we do, Medicaid is clearly better than no coverage."
--Danny McCormick, Harvard Medical School
The Wall Street Journal reminded readers last week that "[w]hen it comes to health policy, governors can make a huge difference." In fact, the WSJ noted, three of 12 gubernatorial elections this year will take place in states that have not expanded Medicaid: Missouri, North Carolina, and Utah.
A separate report (pdf), released this month from the think tank Urban Institute and nonpartisan Robert Wood Johnson Foundation, found that expanding Medicaid "makes economic sense" for the 19 states that have yet to do so.
Last year, when another study showed people with Medicaid insurance have more awareness and better treatment of chronic diseases, Danny McCormick, an associate professor of medicine at Harvard wondered, "With mounting proof that Medicaid improves health, why are politicians refusing to cover their constituents?"
"We need to get everyone covered in a single-payer system," he said at the time, "but until we do, Medicaid is clearly better than no coverage. The Affordable Care Act expanded Medicaid to some states, but not all. We must do better than that if we want to improve the health of all Americans."
Indeed, wrote National Health Law Program executive director Elizabeth Taylor following the Democratic National Convention last month, "Medicaid is our nation's strongest tool to combat health disparities, moving us, albeit slowly, toward a day when all people have the ability to attain the highest level of health."
Dear Common Dreams reader, It’s been nearly 30 years since I co-founded Common Dreams with my late wife, Lina Newhouser. We had the radical notion that journalism should serve the public good, not corporate profits. It was clear to us from the outset what it would take to build such a project. No paid advertisements. No corporate sponsors. No millionaire publisher telling us what to think or do. Many people said we wouldn't last a year, but we proved those doubters wrong. Together with a tremendous team of journalists and dedicated staff, we built an independent media outlet free from the constraints of profits and corporate control. Our mission has always been simple: To inform. To inspire. To ignite change for the common good. Building Common Dreams was not easy. Our survival was never guaranteed. When you take on the most powerful forces—Wall Street greed, fossil fuel industry destruction, Big Tech lobbyists, and uber-rich oligarchs who have spent billions upon billions rigging the economy and democracy in their favor—the only bulwark you have is supporters who believe in your work. But here’s the urgent message from me today. It's never been this bad out there. And it's never been this hard to keep us going. At the very moment Common Dreams is most needed, the threats we face are intensifying. We need your support now more than ever. We don't accept corporate advertising and never will. We don't have a paywall because we don't think people should be blocked from critical news based on their ability to pay. Everything we do is funded by the donations of readers like you. When everyone does the little they can afford, we are strong. But if that support retreats or dries up, so do we. Will you donate now to make sure Common Dreams not only survives but thrives? —Craig Brown, Co-founder |
Bolstering the call for universal coverage and undercutting a key Republican talking point, a new study finds that Medicaid expansion in Arkansas and Kentucky resulted in better healthcare and improved health outcomes among low-income Americans.
The research from the Harvard T.H. Chan School of Public Health shows that two years after Medicaid coverage was expanded under the Affordable Care Act (ACA) in their states, low-income adults in Kentucky and Arkansas received more primary and preventive care, made fewer emergency room visits, had less trouble paying bills, and reported higher quality care and improved health compared with their counterparts in Texas, one of 19 states that did not expand Medicaid.
"Medicaid is our nation's strongest tool to combat health disparities, moving us, albeit slowly, toward a day when all people have the ability to attain the highest level of health."
--Elizabeth Taylor, National Health Law Program
The findings came out Monday in the journal JAMA Internal Medicine.
According to a press statement, lead study author Benjamin Sommers and colleagues surveyed approximately 9,000 low-income adults in Arkansas, Kentucky, and Texas from late 2013 to the end of 2015:
The results showed that, between 2013 and 2015, the uninsured rate dropped from 42 percent to 14 percent in Arkansas and from 40 percent to 9 percent in Kentucky, compared with a much smaller change in Texas (39 percent to 32 percent). Expansion also was associated with significantly increased access to primary care, improved affordability of medications, reduced out-of-pocket spending, reduced likelihood of emergency department visits, and increased outpatient visits. Screening for diabetes, glucose testing among people with diabetes, and regular care for chronic conditions all increased significantly after expansion. Quality of care ratings improved significantly, as did the number of adults reporting excellent health.
The researchers found similar benefits for residents in Kentucky--which expanded traditional Medicaid--and Arkansas, which used federal Medicaid funding to subsidize private insurance, the so-called "private option."
This led Sommers, who teaches at both the Chan School and Harvard Medical School, to declare: "What this means is that it doesn't matter so much how states expand coverage. What matters is whether they expand at all."

Local station WFPL notes:
The results of the new study come as the [Kentucky Gov. Matt] Bevin administration is still sorting through comments on its proposed Medicaid expansion waiver. If approved as-is, it would put in place monthly premiums for individuals earning more than $11,880, co-pays for people earning less than the federal poverty limit, and eliminate default vision and dental coverage for able-bodied adults. Bevin is proposing a 'rewards' account that would let people earn points toward those benefits.
Of Bevin's waiver application, the Kentucky Center for Economic Policy said last month:
The proposed changes will result in fewer Kentuckians covered and decrease health care access, which will ultimately harm the health status of Kentuckians and move the state backwards in its recent health care gains. And while the proposal is framed in terms of increased financial sustainability and reduced costs, it can end up costing the state more overall as it introduces new, expensive and complex administrative burdens, and limits access to the preventative care that improves health. In the end, rolling back Kentucky's historic gains in healthcare coverage would be antithetical to the goals of the Medicaid program [...] and hurt the many Kentuckians who benefit from the Medicaid program in its current form.
"We need to get everyone covered in a single-payer system, but until we do, Medicaid is clearly better than no coverage."
--Danny McCormick, Harvard Medical School
The Wall Street Journal reminded readers last week that "[w]hen it comes to health policy, governors can make a huge difference." In fact, the WSJ noted, three of 12 gubernatorial elections this year will take place in states that have not expanded Medicaid: Missouri, North Carolina, and Utah.
A separate report (pdf), released this month from the think tank Urban Institute and nonpartisan Robert Wood Johnson Foundation, found that expanding Medicaid "makes economic sense" for the 19 states that have yet to do so.
Last year, when another study showed people with Medicaid insurance have more awareness and better treatment of chronic diseases, Danny McCormick, an associate professor of medicine at Harvard wondered, "With mounting proof that Medicaid improves health, why are politicians refusing to cover their constituents?"
"We need to get everyone covered in a single-payer system," he said at the time, "but until we do, Medicaid is clearly better than no coverage. The Affordable Care Act expanded Medicaid to some states, but not all. We must do better than that if we want to improve the health of all Americans."
Indeed, wrote National Health Law Program executive director Elizabeth Taylor following the Democratic National Convention last month, "Medicaid is our nation's strongest tool to combat health disparities, moving us, albeit slowly, toward a day when all people have the ability to attain the highest level of health."
Bolstering the call for universal coverage and undercutting a key Republican talking point, a new study finds that Medicaid expansion in Arkansas and Kentucky resulted in better healthcare and improved health outcomes among low-income Americans.
The research from the Harvard T.H. Chan School of Public Health shows that two years after Medicaid coverage was expanded under the Affordable Care Act (ACA) in their states, low-income adults in Kentucky and Arkansas received more primary and preventive care, made fewer emergency room visits, had less trouble paying bills, and reported higher quality care and improved health compared with their counterparts in Texas, one of 19 states that did not expand Medicaid.
"Medicaid is our nation's strongest tool to combat health disparities, moving us, albeit slowly, toward a day when all people have the ability to attain the highest level of health."
--Elizabeth Taylor, National Health Law Program
The findings came out Monday in the journal JAMA Internal Medicine.
According to a press statement, lead study author Benjamin Sommers and colleagues surveyed approximately 9,000 low-income adults in Arkansas, Kentucky, and Texas from late 2013 to the end of 2015:
The results showed that, between 2013 and 2015, the uninsured rate dropped from 42 percent to 14 percent in Arkansas and from 40 percent to 9 percent in Kentucky, compared with a much smaller change in Texas (39 percent to 32 percent). Expansion also was associated with significantly increased access to primary care, improved affordability of medications, reduced out-of-pocket spending, reduced likelihood of emergency department visits, and increased outpatient visits. Screening for diabetes, glucose testing among people with diabetes, and regular care for chronic conditions all increased significantly after expansion. Quality of care ratings improved significantly, as did the number of adults reporting excellent health.
The researchers found similar benefits for residents in Kentucky--which expanded traditional Medicaid--and Arkansas, which used federal Medicaid funding to subsidize private insurance, the so-called "private option."
This led Sommers, who teaches at both the Chan School and Harvard Medical School, to declare: "What this means is that it doesn't matter so much how states expand coverage. What matters is whether they expand at all."

Local station WFPL notes:
The results of the new study come as the [Kentucky Gov. Matt] Bevin administration is still sorting through comments on its proposed Medicaid expansion waiver. If approved as-is, it would put in place monthly premiums for individuals earning more than $11,880, co-pays for people earning less than the federal poverty limit, and eliminate default vision and dental coverage for able-bodied adults. Bevin is proposing a 'rewards' account that would let people earn points toward those benefits.
Of Bevin's waiver application, the Kentucky Center for Economic Policy said last month:
The proposed changes will result in fewer Kentuckians covered and decrease health care access, which will ultimately harm the health status of Kentuckians and move the state backwards in its recent health care gains. And while the proposal is framed in terms of increased financial sustainability and reduced costs, it can end up costing the state more overall as it introduces new, expensive and complex administrative burdens, and limits access to the preventative care that improves health. In the end, rolling back Kentucky's historic gains in healthcare coverage would be antithetical to the goals of the Medicaid program [...] and hurt the many Kentuckians who benefit from the Medicaid program in its current form.
"We need to get everyone covered in a single-payer system, but until we do, Medicaid is clearly better than no coverage."
--Danny McCormick, Harvard Medical School
The Wall Street Journal reminded readers last week that "[w]hen it comes to health policy, governors can make a huge difference." In fact, the WSJ noted, three of 12 gubernatorial elections this year will take place in states that have not expanded Medicaid: Missouri, North Carolina, and Utah.
A separate report (pdf), released this month from the think tank Urban Institute and nonpartisan Robert Wood Johnson Foundation, found that expanding Medicaid "makes economic sense" for the 19 states that have yet to do so.
Last year, when another study showed people with Medicaid insurance have more awareness and better treatment of chronic diseases, Danny McCormick, an associate professor of medicine at Harvard wondered, "With mounting proof that Medicaid improves health, why are politicians refusing to cover their constituents?"
"We need to get everyone covered in a single-payer system," he said at the time, "but until we do, Medicaid is clearly better than no coverage. The Affordable Care Act expanded Medicaid to some states, but not all. We must do better than that if we want to improve the health of all Americans."
Indeed, wrote National Health Law Program executive director Elizabeth Taylor following the Democratic National Convention last month, "Medicaid is our nation's strongest tool to combat health disparities, moving us, albeit slowly, toward a day when all people have the ability to attain the highest level of health."