
A medic loads a sick nursing home resident with Covid-19 symptoms into an ambulance on August 5, 2020 in Austin, Texas. (Photo: John Moore/Getty Images)
'Bleak Milestone': More Than 100,000 Nursing Home Residents and Staff Killed by Pandemic
Forty percent of all Covid-19 deaths in the United States have occurred in long-term care facilities.
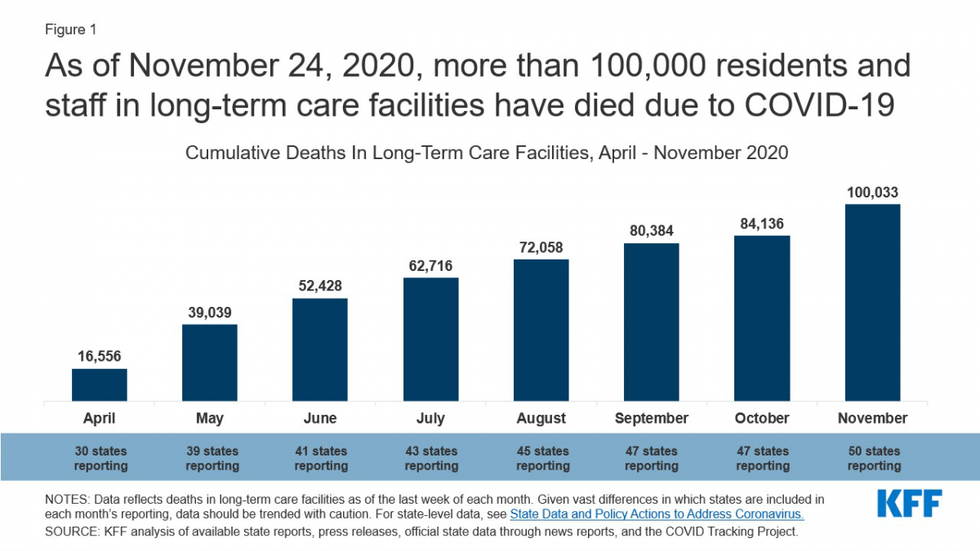
As of the last week of November, Covid-19 has claimed the lives of more than 100,000 people who live and work in long-term care facilities in the United States, according to the Kaiser Family Foundation's latest analysis of state-reported data.
The following chart depicts the growth in Covid-19 deaths among nursing home residents and staff in the U.S. since April. According to the Kaiser Family Foundation (KFF), 40% of the nation's Covid-19 deaths have occurred in long-term care facilities.
"While early action to prevent the spread of coronavirus in long-term care facilities led to strict protocols related to testing, personal protective equipment, and visitor restrictions," KFF pointed out that "several of these measures have been reversed in recent months, and some long-term care facilities continue to report shortages of PPE and staff."
According to physician and public health expert Michael Barnett, 7.7% of the nation's nursing home residents, or one in 13, have now died as a result of Covid-19. "Things have never really gotten better," he tweeted. "Testing is a struggle, PPE and staff are daily challenges."
Soon after reaching the "bleak milestone" of 100,000 pandemic deaths in long-term care facilities, which happened on Tuesday, the U.S. on Thursday experienced a new record-high number of coronavirus-related hospitalizations, as Common Dreams reported earlier Friday.
Millions of Americans have passed through airports in the past week, despite the Centers for Disease Control and Prevention's recommendation against traveling for Thanksgiving. Dr. Anthony Fauci, the nation's top infectious disease expert, does not expect conditions to improve by Christmas and the New Year.
As KFF explained, the predicted "surge in cases after holiday gatherings and increased time indoors due to winter weather... will have ripple effects on hospitals and nursing homes, given the close relationship between community spread and cases in congregate care settings."
The country's Covid-19 death toll surpassed 264,000 on Friday. Meanwhile, Thanksgiving marked the 24th consecutive day of more than 100,000 new daily cases in the U.S.
Given the pandemic's disproportionate impact on the high-risk populations who live and work in long-term care facilities, even more nursing home residents, employees, and their families are expected to be negatively affected by coronavirus as long as the number of infections continues to grow.
"Post-Thanksgiving surges in cases are unlikely to spare this community and will likely lead to an even higher death toll in long-term care facilities," KFF said, "raising questions about whether nursing homes and other facilities are able to protect their residents and, if not, what actions can be taken to mitigate the threat posed by the virus."
As the New York Times reported in June, when the Covid-19 death toll in long-term care facilities was just over 50,000, some critics have argued that the profit-driven nature of the private nursing home industry is the underlying problem, since treating elder care as a commodity rather than a public good can incentivize cost-cutting or money-making measures that put people in harm's way.
An investigation of long-term care facilities in Connecticut, the results of which were published in August, lent credence to that hypothesis. According to the study, "For-profit nursing homes had about 60% more cases and deaths per licensed bed than nonprofit ones," while "larger facilities were hit harder than smaller ones, and... homes serving as part of a chain had worse outcomes," as Reuters reported at the time.
Sen. Sheldon Whitehouse (D-R.I.) noted this week that he and Sen. Bob Casey (D-Pa.) "have a bill to help nursing homes protect their residents and workers from Covid-19."
"It's time," he said, "to pass it."
Urgent. It's never been this bad.
Dear Common Dreams reader, It’s been nearly 30 years since I co-founded Common Dreams with my late wife, Lina Newhouser. We had the radical notion that journalism should serve the public good, not corporate profits. It was clear to us from the outset what it would take to build such a project. No paid advertisements. No corporate sponsors. No millionaire publisher telling us what to think or do. Many people said we wouldn't last a year, but we proved those doubters wrong. Together with a tremendous team of journalists and dedicated staff, we built an independent media outlet free from the constraints of profits and corporate control. Our mission from the outset was simple. To inform. To inspire. To ignite change for the common good. Building Common Dreams was not easy. Our survival was never guaranteed. When you take on the most powerful forces—Wall Street greed, fossil fuel industry destruction, Big Tech lobbyists, and uber-rich oligarchs who have spent billions upon billions rigging the economy and democracy in their favor—the only bulwark you have is supporters who believe in your work. But here’s the urgent message from me today. It’s never been this bad out there. And it’s never been this hard to keep us going. At the very moment Common Dreams is most needed and doing some of its best and most important work, the threats we face are intensifying. Right now, with just two days to go in our Spring Campaign, we're falling short of our make-or-break goal. When everyone does the little they can afford, we are strong. But if that support retreats or dries up, so do we. Can you make a gift right now to make sure Common Dreams not only survives but thrives? There is no backup plan or rainy day fund. There is only you. —Craig Brown, Co-founder |
As of the last week of November, Covid-19 has claimed the lives of more than 100,000 people who live and work in long-term care facilities in the United States, according to the Kaiser Family Foundation's latest analysis of state-reported data.
The following chart depicts the growth in Covid-19 deaths among nursing home residents and staff in the U.S. since April. According to the Kaiser Family Foundation (KFF), 40% of the nation's Covid-19 deaths have occurred in long-term care facilities.

"While early action to prevent the spread of coronavirus in long-term care facilities led to strict protocols related to testing, personal protective equipment, and visitor restrictions," KFF pointed out that "several of these measures have been reversed in recent months, and some long-term care facilities continue to report shortages of PPE and staff."
According to physician and public health expert Michael Barnett, 7.7% of the nation's nursing home residents, or one in 13, have now died as a result of Covid-19. "Things have never really gotten better," he tweeted. "Testing is a struggle, PPE and staff are daily challenges."
Soon after reaching the "bleak milestone" of 100,000 pandemic deaths in long-term care facilities, which happened on Tuesday, the U.S. on Thursday experienced a new record-high number of coronavirus-related hospitalizations, as Common Dreams reported earlier Friday.
Millions of Americans have passed through airports in the past week, despite the Centers for Disease Control and Prevention's recommendation against traveling for Thanksgiving. Dr. Anthony Fauci, the nation's top infectious disease expert, does not expect conditions to improve by Christmas and the New Year.
As KFF explained, the predicted "surge in cases after holiday gatherings and increased time indoors due to winter weather... will have ripple effects on hospitals and nursing homes, given the close relationship between community spread and cases in congregate care settings."
The country's Covid-19 death toll surpassed 264,000 on Friday. Meanwhile, Thanksgiving marked the 24th consecutive day of more than 100,000 new daily cases in the U.S.
Given the pandemic's disproportionate impact on the high-risk populations who live and work in long-term care facilities, even more nursing home residents, employees, and their families are expected to be negatively affected by coronavirus as long as the number of infections continues to grow.
"Post-Thanksgiving surges in cases are unlikely to spare this community and will likely lead to an even higher death toll in long-term care facilities," KFF said, "raising questions about whether nursing homes and other facilities are able to protect their residents and, if not, what actions can be taken to mitigate the threat posed by the virus."
As the New York Times reported in June, when the Covid-19 death toll in long-term care facilities was just over 50,000, some critics have argued that the profit-driven nature of the private nursing home industry is the underlying problem, since treating elder care as a commodity rather than a public good can incentivize cost-cutting or money-making measures that put people in harm's way.
An investigation of long-term care facilities in Connecticut, the results of which were published in August, lent credence to that hypothesis. According to the study, "For-profit nursing homes had about 60% more cases and deaths per licensed bed than nonprofit ones," while "larger facilities were hit harder than smaller ones, and... homes serving as part of a chain had worse outcomes," as Reuters reported at the time.
Sen. Sheldon Whitehouse (D-R.I.) noted this week that he and Sen. Bob Casey (D-Pa.) "have a bill to help nursing homes protect their residents and workers from Covid-19."
"It's time," he said, "to pass it."
As of the last week of November, Covid-19 has claimed the lives of more than 100,000 people who live and work in long-term care facilities in the United States, according to the Kaiser Family Foundation's latest analysis of state-reported data.
The following chart depicts the growth in Covid-19 deaths among nursing home residents and staff in the U.S. since April. According to the Kaiser Family Foundation (KFF), 40% of the nation's Covid-19 deaths have occurred in long-term care facilities.

"While early action to prevent the spread of coronavirus in long-term care facilities led to strict protocols related to testing, personal protective equipment, and visitor restrictions," KFF pointed out that "several of these measures have been reversed in recent months, and some long-term care facilities continue to report shortages of PPE and staff."
According to physician and public health expert Michael Barnett, 7.7% of the nation's nursing home residents, or one in 13, have now died as a result of Covid-19. "Things have never really gotten better," he tweeted. "Testing is a struggle, PPE and staff are daily challenges."
Soon after reaching the "bleak milestone" of 100,000 pandemic deaths in long-term care facilities, which happened on Tuesday, the U.S. on Thursday experienced a new record-high number of coronavirus-related hospitalizations, as Common Dreams reported earlier Friday.
Millions of Americans have passed through airports in the past week, despite the Centers for Disease Control and Prevention's recommendation against traveling for Thanksgiving. Dr. Anthony Fauci, the nation's top infectious disease expert, does not expect conditions to improve by Christmas and the New Year.
As KFF explained, the predicted "surge in cases after holiday gatherings and increased time indoors due to winter weather... will have ripple effects on hospitals and nursing homes, given the close relationship between community spread and cases in congregate care settings."
The country's Covid-19 death toll surpassed 264,000 on Friday. Meanwhile, Thanksgiving marked the 24th consecutive day of more than 100,000 new daily cases in the U.S.
Given the pandemic's disproportionate impact on the high-risk populations who live and work in long-term care facilities, even more nursing home residents, employees, and their families are expected to be negatively affected by coronavirus as long as the number of infections continues to grow.
"Post-Thanksgiving surges in cases are unlikely to spare this community and will likely lead to an even higher death toll in long-term care facilities," KFF said, "raising questions about whether nursing homes and other facilities are able to protect their residents and, if not, what actions can be taken to mitigate the threat posed by the virus."
As the New York Times reported in June, when the Covid-19 death toll in long-term care facilities was just over 50,000, some critics have argued that the profit-driven nature of the private nursing home industry is the underlying problem, since treating elder care as a commodity rather than a public good can incentivize cost-cutting or money-making measures that put people in harm's way.
An investigation of long-term care facilities in Connecticut, the results of which were published in August, lent credence to that hypothesis. According to the study, "For-profit nursing homes had about 60% more cases and deaths per licensed bed than nonprofit ones," while "larger facilities were hit harder than smaller ones, and... homes serving as part of a chain had worse outcomes," as Reuters reported at the time.
Sen. Sheldon Whitehouse (D-R.I.) noted this week that he and Sen. Bob Casey (D-Pa.) "have a bill to help nursing homes protect their residents and workers from Covid-19."
"It's time," he said, "to pass it."

