

SUBSCRIBE TO OUR FREE NEWSLETTER
Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
5
#000000
#FFFFFF
To donate by check, phone, or other method, see our More Ways to Give page.


Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
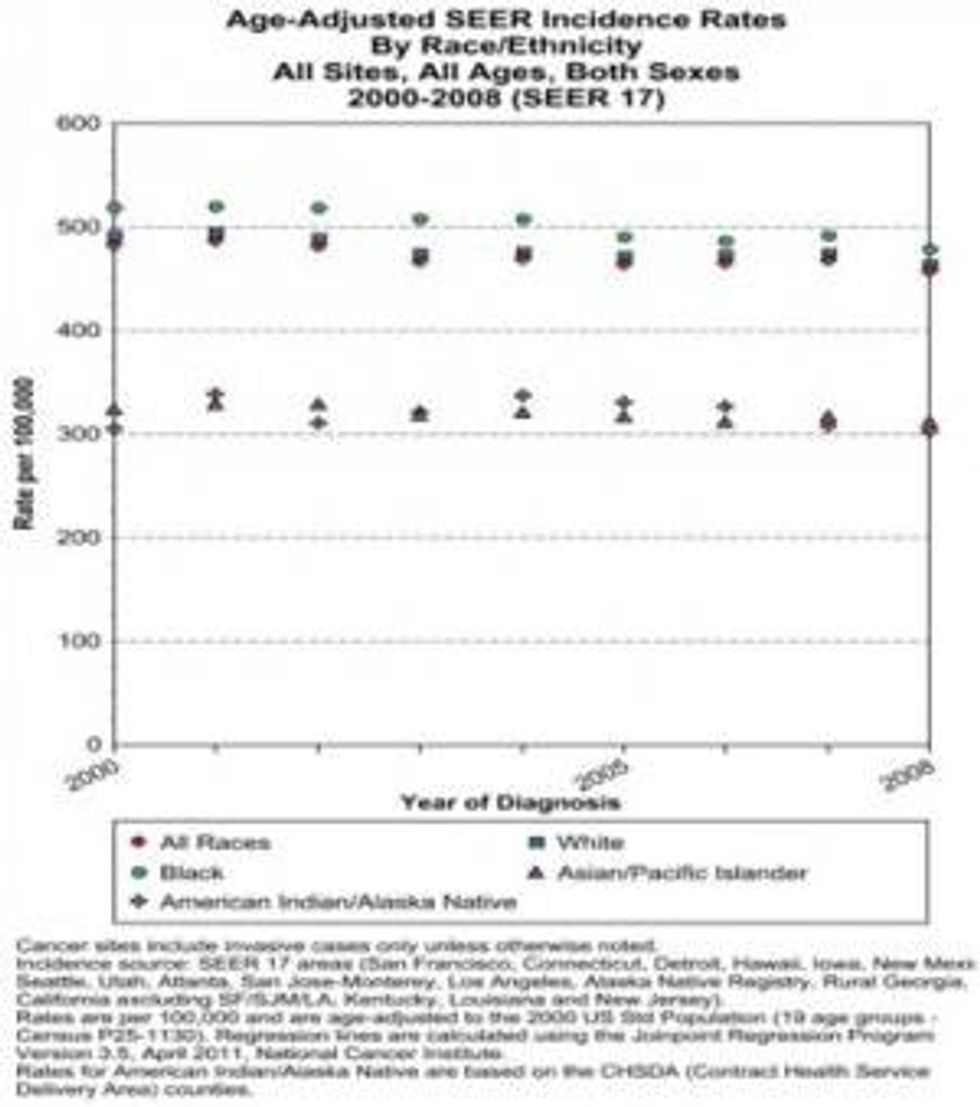
Policy makers must address the disparities in the rates of cancers affecting people of color, ethnic minority, and low-income populations. There is an expanding body of scientific evidence showing the relationship between environmental toxicants and cancer. Low-income populations and people of color have disproportionately high rates of cancers and are more likely to die or be diagnosed at advanced stages of disease. For example the African-American population has the highest overall rate of cancer (Figure 1) and lowest 5-year survival rate cancers (Figure 2). Moreover, African-American men have the highest rate of prostate cancer, and African-American women have the highest mortality rate for breast cancer.
In the United States people of color and racial and ethnic minorities disproportionately live near toxic waste sites. They are also more likely to live in areas of high industrialization, air and water pollution, and work in environments that expose them to cancer causing toxicants. Moreover, this same group of people has a higher rate of exposure and usage of insecticides and pesticides through agriculture work or use in the home. This results in a higher cancer risks then other segments of the population.
Public health studies and research have long documented disparities in health outcomes between ethnic, racial, and socio-economic groups. These disparities are rooted in the environment and in social determinants such as cultural norms, education, income, and stress caused by discriminatory institutional policies and racism. The cumulative effects of these factors are considered risks for cancer and other health problems, adding to the burden of disease for this group of people.
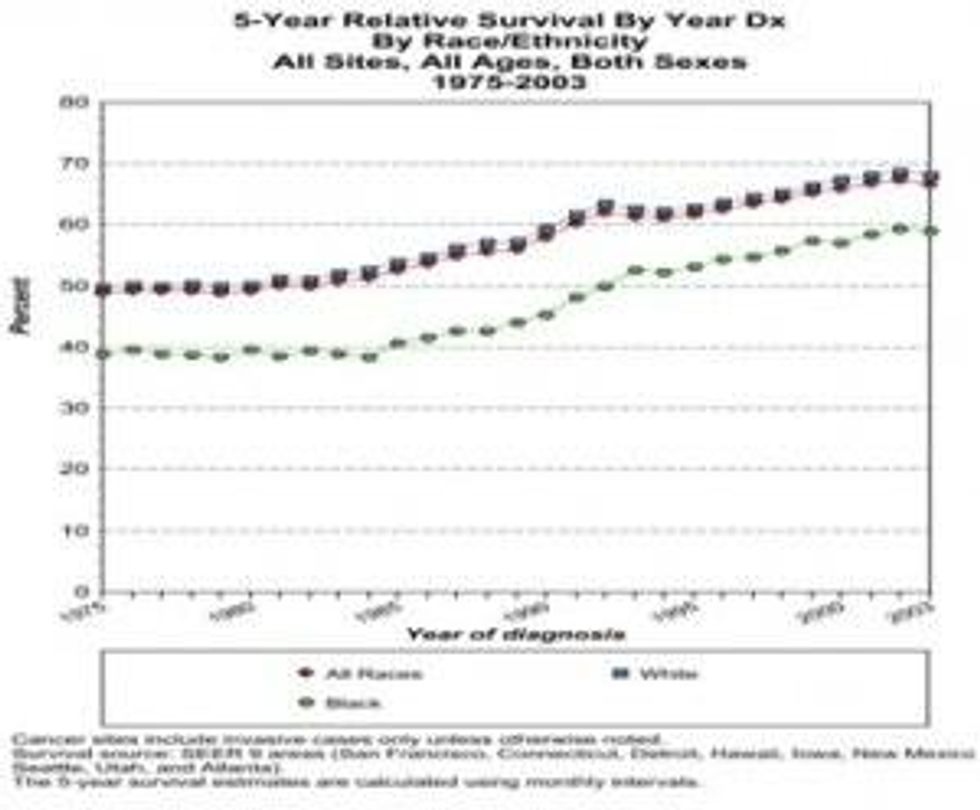
Despite a forty-year history of social change programs, many of these programs work in isolation and have policies that work at cross-purpose; leaving a health disparity gap that has changed little (Figure 2).
The EPA is the process of developing a strategic plan, "Plan EJ 2014," that will incorporate environmental justice into the agency's programs and policies. The overarching goals of the strategic plan are to "protect overburdened polluted communities, empower communities to take action to improve their health and environment, and to collaborate and form partnerships with local, state, tribal and federal organizations." As the implementation of Plan EJ 2014 moves forward, development of the community empowerment strategies focusing on improving health should include the recognition of physicians and other health care professionals as important members of the community.
Physicians are on the front-line of providing care to people who suffer poor health outcomes resulting from exposure to cancer causing environmental toxicants. As such, the role of the physician should be as health care provider and educator who promotes health and awareness about cancer risks and management. Currently, there is a dearth of environmental health training programs in physician training and medical education programs. As a result, many practitioners report not being prepared to counsel patients about environmental health. Collaboration with physician organizations, health care agencies, residency training, and medical schools can ensure incorporation of culturally relevant health education and anticipatory guidance about environmental toxicants into community health programs.
Lastly, as the United States government continues to address the cancer disparities and environmental justice issues present in communities throughout America, the role of physicians should be to translate the science for policy makers. For example, health care providers can educate policy makers through presentations at legislative briefings highlighting the untoward environmental health outcomes of constituents living in their districts, serving on government panels as scientific advisors, or serving as an elected official. Policy makers armed with a broad understanding of science and environmental health issues are able to craft policies to protect communities from the deluge of toxic chemicals inundating minority communities.
Dear Common Dreams reader, It’s been nearly 30 years since I co-founded Common Dreams with my late wife, Lina Newhouser. We had the radical notion that journalism should serve the public good, not corporate profits. It was clear to us from the outset what it would take to build such a project. No paid advertisements. No corporate sponsors. No millionaire publisher telling us what to think or do. Many people said we wouldn't last a year, but we proved those doubters wrong. Together with a tremendous team of journalists and dedicated staff, we built an independent media outlet free from the constraints of profits and corporate control. Our mission has always been simple: To inform. To inspire. To ignite change for the common good. Building Common Dreams was not easy. Our survival was never guaranteed. When you take on the most powerful forces—Wall Street greed, fossil fuel industry destruction, Big Tech lobbyists, and uber-rich oligarchs who have spent billions upon billions rigging the economy and democracy in their favor—the only bulwark you have is supporters who believe in your work. But here’s the urgent message from me today. It's never been this bad out there. And it's never been this hard to keep us going. At the very moment Common Dreams is most needed, the threats we face are intensifying. We need your support now more than ever. We don't accept corporate advertising and never will. We don't have a paywall because we don't think people should be blocked from critical news based on their ability to pay. Everything we do is funded by the donations of readers like you. When everyone does the little they can afford, we are strong. But if that support retreats or dries up, so do we. Will you donate now to make sure Common Dreams not only survives but thrives? —Craig Brown, Co-founder |
Policy makers must address the disparities in the rates of cancers affecting people of color, ethnic minority, and low-income populations. There is an expanding body of scientific evidence showing the relationship between environmental toxicants and cancer. Low-income populations and people of color have disproportionately high rates of cancers and are more likely to die or be diagnosed at advanced stages of disease. For example the African-American population has the highest overall rate of cancer (Figure 1) and lowest 5-year survival rate cancers (Figure 2). Moreover, African-American men have the highest rate of prostate cancer, and African-American women have the highest mortality rate for breast cancer.

In the United States people of color and racial and ethnic minorities disproportionately live near toxic waste sites. They are also more likely to live in areas of high industrialization, air and water pollution, and work in environments that expose them to cancer causing toxicants. Moreover, this same group of people has a higher rate of exposure and usage of insecticides and pesticides through agriculture work or use in the home. This results in a higher cancer risks then other segments of the population.
Public health studies and research have long documented disparities in health outcomes between ethnic, racial, and socio-economic groups. These disparities are rooted in the environment and in social determinants such as cultural norms, education, income, and stress caused by discriminatory institutional policies and racism. The cumulative effects of these factors are considered risks for cancer and other health problems, adding to the burden of disease for this group of people.

Despite a forty-year history of social change programs, many of these programs work in isolation and have policies that work at cross-purpose; leaving a health disparity gap that has changed little (Figure 2).
The EPA is the process of developing a strategic plan, "Plan EJ 2014," that will incorporate environmental justice into the agency's programs and policies. The overarching goals of the strategic plan are to "protect overburdened polluted communities, empower communities to take action to improve their health and environment, and to collaborate and form partnerships with local, state, tribal and federal organizations." As the implementation of Plan EJ 2014 moves forward, development of the community empowerment strategies focusing on improving health should include the recognition of physicians and other health care professionals as important members of the community.
Physicians are on the front-line of providing care to people who suffer poor health outcomes resulting from exposure to cancer causing environmental toxicants. As such, the role of the physician should be as health care provider and educator who promotes health and awareness about cancer risks and management. Currently, there is a dearth of environmental health training programs in physician training and medical education programs. As a result, many practitioners report not being prepared to counsel patients about environmental health. Collaboration with physician organizations, health care agencies, residency training, and medical schools can ensure incorporation of culturally relevant health education and anticipatory guidance about environmental toxicants into community health programs.
Lastly, as the United States government continues to address the cancer disparities and environmental justice issues present in communities throughout America, the role of physicians should be to translate the science for policy makers. For example, health care providers can educate policy makers through presentations at legislative briefings highlighting the untoward environmental health outcomes of constituents living in their districts, serving on government panels as scientific advisors, or serving as an elected official. Policy makers armed with a broad understanding of science and environmental health issues are able to craft policies to protect communities from the deluge of toxic chemicals inundating minority communities.
Policy makers must address the disparities in the rates of cancers affecting people of color, ethnic minority, and low-income populations. There is an expanding body of scientific evidence showing the relationship between environmental toxicants and cancer. Low-income populations and people of color have disproportionately high rates of cancers and are more likely to die or be diagnosed at advanced stages of disease. For example the African-American population has the highest overall rate of cancer (Figure 1) and lowest 5-year survival rate cancers (Figure 2). Moreover, African-American men have the highest rate of prostate cancer, and African-American women have the highest mortality rate for breast cancer.

In the United States people of color and racial and ethnic minorities disproportionately live near toxic waste sites. They are also more likely to live in areas of high industrialization, air and water pollution, and work in environments that expose them to cancer causing toxicants. Moreover, this same group of people has a higher rate of exposure and usage of insecticides and pesticides through agriculture work or use in the home. This results in a higher cancer risks then other segments of the population.
Public health studies and research have long documented disparities in health outcomes between ethnic, racial, and socio-economic groups. These disparities are rooted in the environment and in social determinants such as cultural norms, education, income, and stress caused by discriminatory institutional policies and racism. The cumulative effects of these factors are considered risks for cancer and other health problems, adding to the burden of disease for this group of people.

Despite a forty-year history of social change programs, many of these programs work in isolation and have policies that work at cross-purpose; leaving a health disparity gap that has changed little (Figure 2).
The EPA is the process of developing a strategic plan, "Plan EJ 2014," that will incorporate environmental justice into the agency's programs and policies. The overarching goals of the strategic plan are to "protect overburdened polluted communities, empower communities to take action to improve their health and environment, and to collaborate and form partnerships with local, state, tribal and federal organizations." As the implementation of Plan EJ 2014 moves forward, development of the community empowerment strategies focusing on improving health should include the recognition of physicians and other health care professionals as important members of the community.
Physicians are on the front-line of providing care to people who suffer poor health outcomes resulting from exposure to cancer causing environmental toxicants. As such, the role of the physician should be as health care provider and educator who promotes health and awareness about cancer risks and management. Currently, there is a dearth of environmental health training programs in physician training and medical education programs. As a result, many practitioners report not being prepared to counsel patients about environmental health. Collaboration with physician organizations, health care agencies, residency training, and medical schools can ensure incorporation of culturally relevant health education and anticipatory guidance about environmental toxicants into community health programs.
Lastly, as the United States government continues to address the cancer disparities and environmental justice issues present in communities throughout America, the role of physicians should be to translate the science for policy makers. For example, health care providers can educate policy makers through presentations at legislative briefings highlighting the untoward environmental health outcomes of constituents living in their districts, serving on government panels as scientific advisors, or serving as an elected official. Policy makers armed with a broad understanding of science and environmental health issues are able to craft policies to protect communities from the deluge of toxic chemicals inundating minority communities.