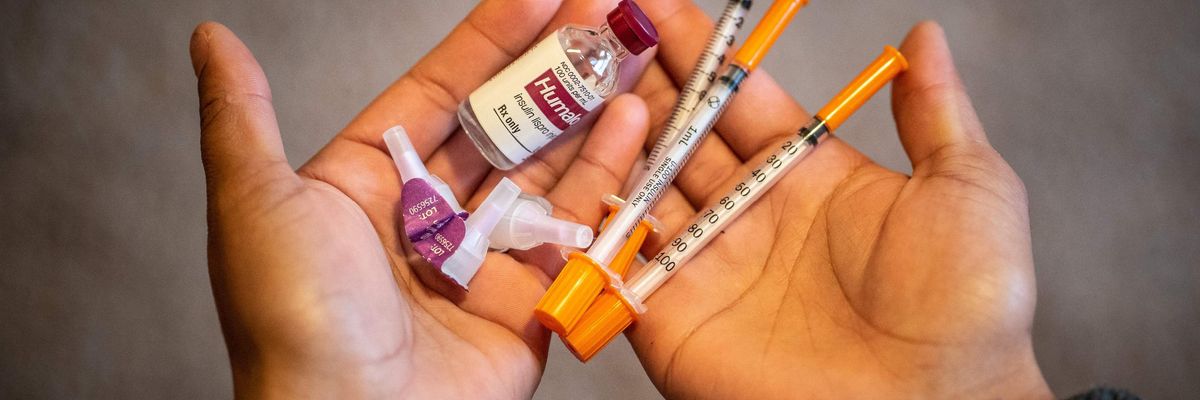
A patient shows her insulin kit on January 17, 2020 in St. Paul, Minnesota. (Photo: Kerem Yucel/AFP via Getty Images)
To Combat Insulin Price Gouging, California Looks Into Generic Drug Production
"Everyone who cares about the future of U.S. domestic policy should pay attention to this effort in California to build a public option for prescription drug manufacturing," said one expert. "Potentially game-changing."
With insulin prices in the United States so astronomical that experts have accused the federal government and pharmaceutical industry of violating human rights, California is exploring a plan to produce its own generic version of the lifesaving medicine and make it accessible to millions of people with diabetes.
"Everyone who cares about the future of U.S. domestic policy should pay attention to this effort in California to build a public option for prescription drug manufacturing," Steph Sterling, vice president of the Roosevelt Institute, a progressive think tank, said Tuesday.
As Kaiser Health News reported, California is "attempting to achieve what no other state has done: produce its own brand of generic insulin and sell it at below-market prices to people with diabetes."
California Democratic Gov. Gavin Newsom "is asking state lawmakers to pump $100 million into an ambitious initiative to launch California's generic drug label, CalRx, and begin producing insulin in the next few years," the news outlet reported. "The state is also working to identify other generic drugs it could bring to market, targeting those that are expensive or in short supply."
An estimated four million Californians have been diagnosed with diabetes, a disease that can wreak havoc on organs, eyesight, and limbs if left unmanaged.
Just three pharmaceutical corporations control the nation's lucrative insulin market, however, so the century-old drug ranges in price from $300 to $400 per vial without insurance. Due to this rampant price gouging and the widespread lack of coverage under a for-profit healthcare system, one-quarter of Californians who rely on insulin to live with diabetes cannot afford it. Corporate profiteering is forcing many people to ration the drug or go without it, with deadly consequences.
Related Content

'Our System Kills People': 27-Year-Old Diabetic Man Latest to Die in US Amid Skyrocketing Cost of Insulin
Taking on Big Pharma's monopoly power requires government intervention, Newsom said last month. He added that California--home to 40 million residents and the world's fifth-largest economy--has the clout to reduce sky-high drug prices.
Challenges remain, however, as KHN reported:
State health officials are still negotiating a contract with a drug manufacturer to make and distribute insulin and have not answered key questions such as how cheaply insulin could be produced and what patients would pay. To be successful, California--and the company it partners with--must navigate a complicated pharmaceutical distribution system that relies not only on drug manufacturers but also middleman companies that work hand in hand with health insurers. Those companies, known as pharmacy benefit managers, negotiate with manufacturers on behalf of insurers for rebates and discounts on drugs--but insurers don't always pass those savings on to consumers.
[...]
The Newsom administration thinks state-made insulin could cut some insurers' spending on the drug as much as 70%--savings it hopes would trickle down to consumers. But "there is no guarantee" that the administration's predictions of dramatic savings or wide distribution of insulin will materialize, state Assembly member Blanca Rubio (D-48) said at [a legislative hearing in May]. "Who is going to write the prescriptions for this magic insulin?" she asked. "Hope is not a strategy. I'm not hearing any strategies as to how this is going to become available."
A U.S. Senate investigation published last year found that the price of a long-acting insulin pen made by Novo Nordisk shot up 52% from 2014 to 2019 and that the price of Sanofi's rapid-acting pen surged by roughly 70%. The probe attributed the cost hikes to the drugmakers as well as pharmacy benefit managers, criticizing them for artificially inflating insulin prices.
When contacted for comment, "the trade associations that represent brand-name drugmakers, pharmacy benefit managers, and California health insurers blamed one another for the increase in prices," KHN reported.
Diabetes affects more than 37 million U.S. adults and is the country's seventh leading cause of death, according to the U.S. Centers for Disease Control and Prevention.
The U.S. House of Representatives recently passed legislation that would cap insulin copayments at $35 a month. But critics, including some Democratic lawmakers who ultimately voted for the bill, pointed out that it would not bring down actual insulin prices, meaning that countless diabetes patients who lack private insurance or Medicare would not benefit from the measure even if it were enacted.
The bill's path through the evenly split U.S. Senate remains unclear, given that the 60-vote filibuster gives the Republican minority veto power over most legislation. Corporate-backed Senate Democrats such as Kyrsten Sinema (Ariz.) and Joe Manchin (W.Va.)--whose daughter Heather Bresch played a direct role in an EpiPen price gouging scandal--have refused to suspend the upper chamber's gridlock-enhancing rule.
The void left by congressional inaction gives California's proposal even greater stakes.
KHN explained that "under Newsom's plan, generic forms of insulin--known as 'biosimilars' because they are made with living cells and mimic brand-name drugs on the market--would be widely available to insured and uninsured Californians."
"If Newsom's $100 million initiative is approved by lawmakers this summer," the news outlet reported, "the state would use that money to contract with an established drugmaker to begin supplying CalRx insulin while the state constructs its own manufacturing facility, also in partnership with a drugmaker."
"The administration is currently negotiating with drug companies that can produce a reliable supply of insulin under a no-bid contract, but no partnership has been formalized," KHN noted. "The insulin would be branded with images associated with the state, such as the 'California Golden Bear.' And... the packaging could boast that the lower-priced insulin was brought to patients by state government."
Sterling, for her part, called California's approach "potentially game-changing."
Urgent. It's never been this bad.
Dear Common Dreams reader, It’s been nearly 30 years since I co-founded Common Dreams with my late wife, Lina Newhouser. We had the radical notion that journalism should serve the public good, not corporate profits. It was clear to us from the outset what it would take to build such a project. No paid advertisements. No corporate sponsors. No millionaire publisher telling us what to think or do. Many people said we wouldn't last a year, but we proved those doubters wrong. Together with a tremendous team of journalists and dedicated staff, we built an independent media outlet free from the constraints of profits and corporate control. Our mission from the outset was simple. To inform. To inspire. To ignite change for the common good. Building Common Dreams was not easy. Our survival was never guaranteed. When you take on the most powerful forces—Wall Street greed, fossil fuel industry destruction, Big Tech lobbyists, and uber-rich oligarchs who have spent billions upon billions rigging the economy and democracy in their favor—the only bulwark you have is supporters who believe in your work. But here’s the urgent message from me today. It’s never been this bad out there. And it’s never been this hard to keep us going. At the very moment Common Dreams is most needed and doing some of its best and most important work, the threats we face are intensifying. Right now, with just four days to go in our Spring Campaign, we are not even halfway to our goal. When everyone does the little they can afford, we are strong. But if that support retreats or dries up, so do we. Can you make a gift right now to make sure Common Dreams not only survives but thrives? There is no backup plan or rainy day fund. There is only you. —Craig Brown, Co-founder |
With insulin prices in the United States so astronomical that experts have accused the federal government and pharmaceutical industry of violating human rights, California is exploring a plan to produce its own generic version of the lifesaving medicine and make it accessible to millions of people with diabetes.
"Everyone who cares about the future of U.S. domestic policy should pay attention to this effort in California to build a public option for prescription drug manufacturing," Steph Sterling, vice president of the Roosevelt Institute, a progressive think tank, said Tuesday.
As Kaiser Health News reported, California is "attempting to achieve what no other state has done: produce its own brand of generic insulin and sell it at below-market prices to people with diabetes."
California Democratic Gov. Gavin Newsom "is asking state lawmakers to pump $100 million into an ambitious initiative to launch California's generic drug label, CalRx, and begin producing insulin in the next few years," the news outlet reported. "The state is also working to identify other generic drugs it could bring to market, targeting those that are expensive or in short supply."
An estimated four million Californians have been diagnosed with diabetes, a disease that can wreak havoc on organs, eyesight, and limbs if left unmanaged.
Just three pharmaceutical corporations control the nation's lucrative insulin market, however, so the century-old drug ranges in price from $300 to $400 per vial without insurance. Due to this rampant price gouging and the widespread lack of coverage under a for-profit healthcare system, one-quarter of Californians who rely on insulin to live with diabetes cannot afford it. Corporate profiteering is forcing many people to ration the drug or go without it, with deadly consequences.
Related Content

'Our System Kills People': 27-Year-Old Diabetic Man Latest to Die in US Amid Skyrocketing Cost of Insulin
Taking on Big Pharma's monopoly power requires government intervention, Newsom said last month. He added that California--home to 40 million residents and the world's fifth-largest economy--has the clout to reduce sky-high drug prices.
Challenges remain, however, as KHN reported:
State health officials are still negotiating a contract with a drug manufacturer to make and distribute insulin and have not answered key questions such as how cheaply insulin could be produced and what patients would pay. To be successful, California--and the company it partners with--must navigate a complicated pharmaceutical distribution system that relies not only on drug manufacturers but also middleman companies that work hand in hand with health insurers. Those companies, known as pharmacy benefit managers, negotiate with manufacturers on behalf of insurers for rebates and discounts on drugs--but insurers don't always pass those savings on to consumers.
[...]
The Newsom administration thinks state-made insulin could cut some insurers' spending on the drug as much as 70%--savings it hopes would trickle down to consumers. But "there is no guarantee" that the administration's predictions of dramatic savings or wide distribution of insulin will materialize, state Assembly member Blanca Rubio (D-48) said at [a legislative hearing in May]. "Who is going to write the prescriptions for this magic insulin?" she asked. "Hope is not a strategy. I'm not hearing any strategies as to how this is going to become available."
A U.S. Senate investigation published last year found that the price of a long-acting insulin pen made by Novo Nordisk shot up 52% from 2014 to 2019 and that the price of Sanofi's rapid-acting pen surged by roughly 70%. The probe attributed the cost hikes to the drugmakers as well as pharmacy benefit managers, criticizing them for artificially inflating insulin prices.
When contacted for comment, "the trade associations that represent brand-name drugmakers, pharmacy benefit managers, and California health insurers blamed one another for the increase in prices," KHN reported.
Diabetes affects more than 37 million U.S. adults and is the country's seventh leading cause of death, according to the U.S. Centers for Disease Control and Prevention.
The U.S. House of Representatives recently passed legislation that would cap insulin copayments at $35 a month. But critics, including some Democratic lawmakers who ultimately voted for the bill, pointed out that it would not bring down actual insulin prices, meaning that countless diabetes patients who lack private insurance or Medicare would not benefit from the measure even if it were enacted.
The bill's path through the evenly split U.S. Senate remains unclear, given that the 60-vote filibuster gives the Republican minority veto power over most legislation. Corporate-backed Senate Democrats such as Kyrsten Sinema (Ariz.) and Joe Manchin (W.Va.)--whose daughter Heather Bresch played a direct role in an EpiPen price gouging scandal--have refused to suspend the upper chamber's gridlock-enhancing rule.
The void left by congressional inaction gives California's proposal even greater stakes.
KHN explained that "under Newsom's plan, generic forms of insulin--known as 'biosimilars' because they are made with living cells and mimic brand-name drugs on the market--would be widely available to insured and uninsured Californians."
"If Newsom's $100 million initiative is approved by lawmakers this summer," the news outlet reported, "the state would use that money to contract with an established drugmaker to begin supplying CalRx insulin while the state constructs its own manufacturing facility, also in partnership with a drugmaker."
"The administration is currently negotiating with drug companies that can produce a reliable supply of insulin under a no-bid contract, but no partnership has been formalized," KHN noted. "The insulin would be branded with images associated with the state, such as the 'California Golden Bear.' And... the packaging could boast that the lower-priced insulin was brought to patients by state government."
Sterling, for her part, called California's approach "potentially game-changing."
With insulin prices in the United States so astronomical that experts have accused the federal government and pharmaceutical industry of violating human rights, California is exploring a plan to produce its own generic version of the lifesaving medicine and make it accessible to millions of people with diabetes.
"Everyone who cares about the future of U.S. domestic policy should pay attention to this effort in California to build a public option for prescription drug manufacturing," Steph Sterling, vice president of the Roosevelt Institute, a progressive think tank, said Tuesday.
As Kaiser Health News reported, California is "attempting to achieve what no other state has done: produce its own brand of generic insulin and sell it at below-market prices to people with diabetes."
California Democratic Gov. Gavin Newsom "is asking state lawmakers to pump $100 million into an ambitious initiative to launch California's generic drug label, CalRx, and begin producing insulin in the next few years," the news outlet reported. "The state is also working to identify other generic drugs it could bring to market, targeting those that are expensive or in short supply."
An estimated four million Californians have been diagnosed with diabetes, a disease that can wreak havoc on organs, eyesight, and limbs if left unmanaged.
Just three pharmaceutical corporations control the nation's lucrative insulin market, however, so the century-old drug ranges in price from $300 to $400 per vial without insurance. Due to this rampant price gouging and the widespread lack of coverage under a for-profit healthcare system, one-quarter of Californians who rely on insulin to live with diabetes cannot afford it. Corporate profiteering is forcing many people to ration the drug or go without it, with deadly consequences.
Related Content

'Our System Kills People': 27-Year-Old Diabetic Man Latest to Die in US Amid Skyrocketing Cost of Insulin
Taking on Big Pharma's monopoly power requires government intervention, Newsom said last month. He added that California--home to 40 million residents and the world's fifth-largest economy--has the clout to reduce sky-high drug prices.
Challenges remain, however, as KHN reported:
State health officials are still negotiating a contract with a drug manufacturer to make and distribute insulin and have not answered key questions such as how cheaply insulin could be produced and what patients would pay. To be successful, California--and the company it partners with--must navigate a complicated pharmaceutical distribution system that relies not only on drug manufacturers but also middleman companies that work hand in hand with health insurers. Those companies, known as pharmacy benefit managers, negotiate with manufacturers on behalf of insurers for rebates and discounts on drugs--but insurers don't always pass those savings on to consumers.
[...]
The Newsom administration thinks state-made insulin could cut some insurers' spending on the drug as much as 70%--savings it hopes would trickle down to consumers. But "there is no guarantee" that the administration's predictions of dramatic savings or wide distribution of insulin will materialize, state Assembly member Blanca Rubio (D-48) said at [a legislative hearing in May]. "Who is going to write the prescriptions for this magic insulin?" she asked. "Hope is not a strategy. I'm not hearing any strategies as to how this is going to become available."
A U.S. Senate investigation published last year found that the price of a long-acting insulin pen made by Novo Nordisk shot up 52% from 2014 to 2019 and that the price of Sanofi's rapid-acting pen surged by roughly 70%. The probe attributed the cost hikes to the drugmakers as well as pharmacy benefit managers, criticizing them for artificially inflating insulin prices.
When contacted for comment, "the trade associations that represent brand-name drugmakers, pharmacy benefit managers, and California health insurers blamed one another for the increase in prices," KHN reported.
Diabetes affects more than 37 million U.S. adults and is the country's seventh leading cause of death, according to the U.S. Centers for Disease Control and Prevention.
The U.S. House of Representatives recently passed legislation that would cap insulin copayments at $35 a month. But critics, including some Democratic lawmakers who ultimately voted for the bill, pointed out that it would not bring down actual insulin prices, meaning that countless diabetes patients who lack private insurance or Medicare would not benefit from the measure even if it were enacted.
The bill's path through the evenly split U.S. Senate remains unclear, given that the 60-vote filibuster gives the Republican minority veto power over most legislation. Corporate-backed Senate Democrats such as Kyrsten Sinema (Ariz.) and Joe Manchin (W.Va.)--whose daughter Heather Bresch played a direct role in an EpiPen price gouging scandal--have refused to suspend the upper chamber's gridlock-enhancing rule.
The void left by congressional inaction gives California's proposal even greater stakes.
KHN explained that "under Newsom's plan, generic forms of insulin--known as 'biosimilars' because they are made with living cells and mimic brand-name drugs on the market--would be widely available to insured and uninsured Californians."
"If Newsom's $100 million initiative is approved by lawmakers this summer," the news outlet reported, "the state would use that money to contract with an established drugmaker to begin supplying CalRx insulin while the state constructs its own manufacturing facility, also in partnership with a drugmaker."
"The administration is currently negotiating with drug companies that can produce a reliable supply of insulin under a no-bid contract, but no partnership has been formalized," KHN noted. "The insulin would be branded with images associated with the state, such as the 'California Golden Bear.' And... the packaging could boast that the lower-priced insulin was brought to patients by state government."
Sterling, for her part, called California's approach "potentially game-changing."

