

SUBSCRIBE TO OUR FREE NEWSLETTER
Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
5
#000000
#FFFFFF
To donate by check, phone, or other method, see our More Ways to Give page.


Daily news & progressive opinion—funded by the people, not the corporations—delivered straight to your inbox.
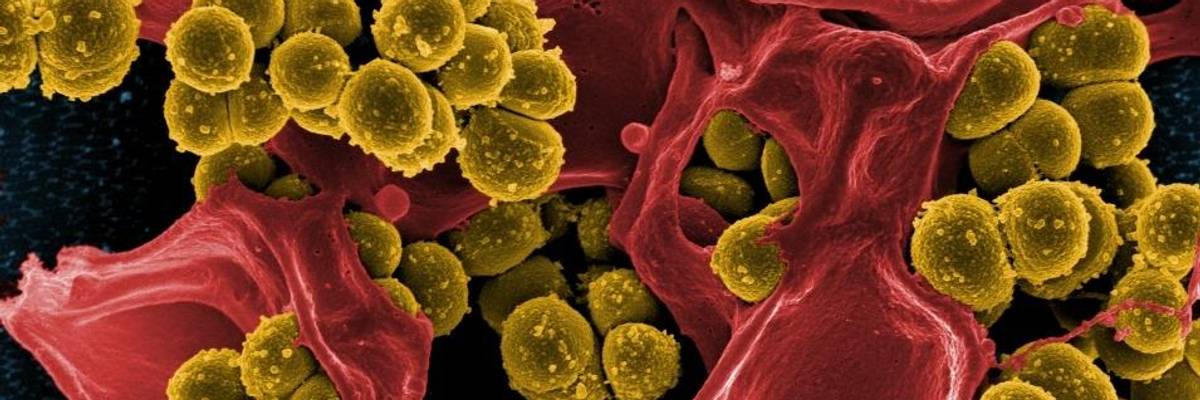
Micrograph of Methicillin-Resistant Staphylococcus aureus (MRSA) (Photo: NIAID)
Adding to mounting concerns about widespread antibiotic resistance, U.S. public health officials detected more than 220 cases of what they described as "nightmare bacteria" across more than half the country last year, according to a new government report.
In just nine months of surveillance during 2017, the Centers for Disease Control and Prevention (CDC) found "nightmare bacteria" with "unusual" resistance in 27 states, fueling the agency's warnings that "antibiotic-resistant germs can spread like wildfire."
The CDC considers antibiotic-resistant germs "unusual" if they are: resistant to all or most antibiotics; uncommon in a geographic area or the U.S.; or have genes that allow them to spread their resistance to other germs.
These "dangerous pathogens, hiding in plain sight...can cause infections that are difficult or impossible to treat," explained CDC principal deputy director Dr. Anne Schuchat. "Taking a terrible human toll, two million Americans get infections from antibiotic resistance and 23,000 die from those infections each year."
In response to this growing threat to public health, the CDC has launched a containment strategy that includes a nationwide lab network for identifying new and "unusual" antibiotic-resistant germs.
Last year, as the CDC's new Vital Sign report outlines, the agency's nationwide network of labs tested 5,776 samples for "genes that were highly resistant or rare with special resistance that could spread."
"Of the 5,776, about one in four of the bacteria had a gene that helps it spread its resistance. And there were 221 instances of an especially rare resistance gene," Schuchat told reporters in a press briefing.
Patients who had contracted the "nightmare bateria" were at hospitals as well as healthcare facilities such as nursing homes. They were battling pneumonia, urinary tract infections, blood stream infections, and other types of infections. Although the report did not detail how many cases were fatal, Schuchat noted past research suggests "up to 50 percent can result in death."
While Schuchat admitted that the number of "nightmare bacteria" cases was higher than she expected, she added, "We hope though that this won't be an inevitable march upward, but that by finding them early when there's only one in the facility we can stop this from becoming very, very common."
The CDC containment strategy calls for a coordinated effort among healthcare facilities, labs, health departments, and CDC's lab network to rapidly identify resistance; implement infection control assessments; test patients who are not showing symptoms but may carry and spread the germ; and continue infection control assessments until the spread of that particular germ has stopped.
"Health departments using the approach have conducted infection control assessments and colonization screenings within 48 hours of finding unusual resistance and have reported no further transmission during follow-up over several weeks," the agency said in a statement. For the superbug CRE, "estimates show that the containment strategy would prevent as many as 1,600 new infections in three years in a single state--a 76 percent reduction."
Dear Common Dreams reader, It’s been nearly 30 years since I co-founded Common Dreams with my late wife, Lina Newhouser. We had the radical notion that journalism should serve the public good, not corporate profits. It was clear to us from the outset what it would take to build such a project. No paid advertisements. No corporate sponsors. No millionaire publisher telling us what to think or do. Many people said we wouldn't last a year, but we proved those doubters wrong. Together with a tremendous team of journalists and dedicated staff, we built an independent media outlet free from the constraints of profits and corporate control. Our mission has always been simple: To inform. To inspire. To ignite change for the common good. Building Common Dreams was not easy. Our survival was never guaranteed. When you take on the most powerful forces—Wall Street greed, fossil fuel industry destruction, Big Tech lobbyists, and uber-rich oligarchs who have spent billions upon billions rigging the economy and democracy in their favor—the only bulwark you have is supporters who believe in your work. But here’s the urgent message from me today. It's never been this bad out there. And it's never been this hard to keep us going. At the very moment Common Dreams is most needed, the threats we face are intensifying. We need your support now more than ever. We don't accept corporate advertising and never will. We don't have a paywall because we don't think people should be blocked from critical news based on their ability to pay. Everything we do is funded by the donations of readers like you. When everyone does the little they can afford, we are strong. But if that support retreats or dries up, so do we. Will you donate now to make sure Common Dreams not only survives but thrives? —Craig Brown, Co-founder |
Adding to mounting concerns about widespread antibiotic resistance, U.S. public health officials detected more than 220 cases of what they described as "nightmare bacteria" across more than half the country last year, according to a new government report.
In just nine months of surveillance during 2017, the Centers for Disease Control and Prevention (CDC) found "nightmare bacteria" with "unusual" resistance in 27 states, fueling the agency's warnings that "antibiotic-resistant germs can spread like wildfire."
The CDC considers antibiotic-resistant germs "unusual" if they are: resistant to all or most antibiotics; uncommon in a geographic area or the U.S.; or have genes that allow them to spread their resistance to other germs.
These "dangerous pathogens, hiding in plain sight...can cause infections that are difficult or impossible to treat," explained CDC principal deputy director Dr. Anne Schuchat. "Taking a terrible human toll, two million Americans get infections from antibiotic resistance and 23,000 die from those infections each year."
In response to this growing threat to public health, the CDC has launched a containment strategy that includes a nationwide lab network for identifying new and "unusual" antibiotic-resistant germs.
Last year, as the CDC's new Vital Sign report outlines, the agency's nationwide network of labs tested 5,776 samples for "genes that were highly resistant or rare with special resistance that could spread."
"Of the 5,776, about one in four of the bacteria had a gene that helps it spread its resistance. And there were 221 instances of an especially rare resistance gene," Schuchat told reporters in a press briefing.
Patients who had contracted the "nightmare bateria" were at hospitals as well as healthcare facilities such as nursing homes. They were battling pneumonia, urinary tract infections, blood stream infections, and other types of infections. Although the report did not detail how many cases were fatal, Schuchat noted past research suggests "up to 50 percent can result in death."
While Schuchat admitted that the number of "nightmare bacteria" cases was higher than she expected, she added, "We hope though that this won't be an inevitable march upward, but that by finding them early when there's only one in the facility we can stop this from becoming very, very common."
The CDC containment strategy calls for a coordinated effort among healthcare facilities, labs, health departments, and CDC's lab network to rapidly identify resistance; implement infection control assessments; test patients who are not showing symptoms but may carry and spread the germ; and continue infection control assessments until the spread of that particular germ has stopped.
"Health departments using the approach have conducted infection control assessments and colonization screenings within 48 hours of finding unusual resistance and have reported no further transmission during follow-up over several weeks," the agency said in a statement. For the superbug CRE, "estimates show that the containment strategy would prevent as many as 1,600 new infections in three years in a single state--a 76 percent reduction."
Adding to mounting concerns about widespread antibiotic resistance, U.S. public health officials detected more than 220 cases of what they described as "nightmare bacteria" across more than half the country last year, according to a new government report.
In just nine months of surveillance during 2017, the Centers for Disease Control and Prevention (CDC) found "nightmare bacteria" with "unusual" resistance in 27 states, fueling the agency's warnings that "antibiotic-resistant germs can spread like wildfire."
The CDC considers antibiotic-resistant germs "unusual" if they are: resistant to all or most antibiotics; uncommon in a geographic area or the U.S.; or have genes that allow them to spread their resistance to other germs.
These "dangerous pathogens, hiding in plain sight...can cause infections that are difficult or impossible to treat," explained CDC principal deputy director Dr. Anne Schuchat. "Taking a terrible human toll, two million Americans get infections from antibiotic resistance and 23,000 die from those infections each year."
In response to this growing threat to public health, the CDC has launched a containment strategy that includes a nationwide lab network for identifying new and "unusual" antibiotic-resistant germs.
Last year, as the CDC's new Vital Sign report outlines, the agency's nationwide network of labs tested 5,776 samples for "genes that were highly resistant or rare with special resistance that could spread."
"Of the 5,776, about one in four of the bacteria had a gene that helps it spread its resistance. And there were 221 instances of an especially rare resistance gene," Schuchat told reporters in a press briefing.
Patients who had contracted the "nightmare bateria" were at hospitals as well as healthcare facilities such as nursing homes. They were battling pneumonia, urinary tract infections, blood stream infections, and other types of infections. Although the report did not detail how many cases were fatal, Schuchat noted past research suggests "up to 50 percent can result in death."
While Schuchat admitted that the number of "nightmare bacteria" cases was higher than she expected, she added, "We hope though that this won't be an inevitable march upward, but that by finding them early when there's only one in the facility we can stop this from becoming very, very common."
The CDC containment strategy calls for a coordinated effort among healthcare facilities, labs, health departments, and CDC's lab network to rapidly identify resistance; implement infection control assessments; test patients who are not showing symptoms but may carry and spread the germ; and continue infection control assessments until the spread of that particular germ has stopped.
"Health departments using the approach have conducted infection control assessments and colonization screenings within 48 hours of finding unusual resistance and have reported no further transmission during follow-up over several weeks," the agency said in a statement. For the superbug CRE, "estimates show that the containment strategy would prevent as many as 1,600 new infections in three years in a single state--a 76 percent reduction."